“The Next Big Thing.” “2016’s Trending Skincare Treatment.” “Our New Favorite Skincare Procedure.” Even if you didn’t see these headlines, you have likely experienced an increase in patients asking about microneedling. Although the procedure has been around for decades, it has recently become a media darling.
There’s no single significant event that explains the surge in interest. But physicians have seen growing evidence that inducing channels of dermal injury whether by laser or needles stimulates collagen regeneration. Improved microneedling devices as well as better treatment protocols, including adjuncts such as platelet-rich plasma (PRP), and the availability of more professional training may also be playing a role.
Perhaps the best explanation for the increased popularity of medical microneedling is the growing number of patients seeking affordable skincare treatments that offer visible results—a micro-needling session typically costs about a quarter of what patients pay per laser treatment.
“One of the disadvantages of medical microneedling is that patients often confuse it with roller-type microneedling employed by estheticians,” says Tina S. Alster, MD, director of the Washington Institute of Dermatologic Laser Surgery and clinical professor of dermatology at Georgetown University Hospital in Washington, D.C., who uses medical microneedling in patients of every skin phototype for a variety of indications.
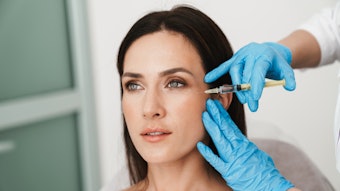
Medical microneedling devices do not employ rollers; instead they feature a motor that rapidly applies a needle configuration in a stamping fashion to the skin. Practitioners can vary the speed and depth of penetration.
According to the U.S. Food and Drug Administration (FDA), any procedure using a needle more than 0.2mm in length is a medical procedure, but in a few states nurses and other ancillary providers can still perform microneedling treatments using devices with needles up to 1.5mm in length.
It is considered safer than many other aesthetic procedures, as the majority of adverse events—including prolonged redness, dermatitis and infection—have been traced to two causes: the application of inappropriate topical products and improper patient selection. There are some basic contraindications for microneedling such as active skin infection, open wounds and wound healing/collagen disorders. Some physicians also screen patients for recent sun exposure (or planned sun exposure within a week of treatment) or recent ablative skin resurfacing procedures.
Photo copyright Getty Images.
[pagebreak]
“Our experience with microneedling is that it is a powerful tool for skin rejuvenation, particularly off the face, and especially in conjunction with PRP,” says Garry R. Lee, MD, director of Look Younger MD in Henderson, Nevada. “It smooths fine scars, helps with discolorations, is moderately effective for skin tightening and is potent for adding luminosity. It helps—but does not remove—most wrinkles, and appears to be useful for pore size reduction. Microneedling is much more affordable for the practitioner than most conventional laser, radiofrequency (RF) or plasma energy treatments, and can deliver comparable results to our observation. This is why you often hear it described as the ‘poor man’s laser,’ though I would consider it the ‘wise man’s laser.’”
The Procedure
“Microneedling is safe to use in patients with any skin phototype. It is a quick treatment with fast postoperative recovery and limited side effects,” says Dr. Alster, who uses either a Collagen P. I.N. (Induction Therapies) or an Eclipse MicroPen in her practice.
Treatment areas are cleansed and prepped with alcohol pads before application of topical anesthetic, either 30% lidocaine or BLT (benzocaine 20%/lidocaine 6%/tetracaine 4%). After 30 to 45 minutes, the anesthetic is removed and the skin is again prepped with alcohol pads.
Treatment times vary based on the area involved: “From about 5 minutes for specific areas like the upper lip to as much as 30 minutes for striae on the body,” says Dr. Alster. “We recommend an average of three sessions at monthly intervals.”
Johnson C. Lee, MD, a plastic surgeon practicing in Beverly Hills, California, is able to treat the whole face in 15 to 20 minutes. “We recommend two to three initial sessions at six-week intervals to start, followed by annual maintenance visits for most patients. Scars can take 10 minutes or less. I have used the SkinPen (Bellus Medical) and the Dermapen, both of which work well. Needle lengths vary from 0.5mm to 2.5mm and can be adjusted, depending on the area being treated. I prefer to use the maximum depth tolerated by the patient, particularly with scar treatments. I will switch to more superficial depths (< 2mm) for additional passes or in more sensitive areas, such as the forehead and jawline, as well as for patients who have more sensitive skin,” he says.
While downtime is limited to a day or two, “patients should expect significant redness in the treatment area, particularly 24 hours later,” says Dr. Garry Lee. “We have yet to have one, but patients should watch for signs and symptoms of infection, including redness, pain, warmth and swelling. We instruct patients to avoid applying creams, lotions, sunblock or makeup for at least eight hours post treatment. After eight hours, patients may wash the treated area with a gentle cleanser, such as Cetaphil, followed by a gentle moisturizer, such as TNS Ceramide Cream.”
Dale Isaacson, MD, and Marilyn Berzin, MD, of DC Derm Docs in Washington, D.C., ask patients not to apply makeup on the day of the procedure and recommend avoiding topical medications for three days. They do suggest patients begin using a sunscreen the day after the procedure and continue until all redness is gone.
Photo copyright Getty Images.
[pagebreak]
Dr. Alster advises her patients to apply a soothing balm for a day or two, avoid makeup or other skin preparations for two to three days, and avoid sun exposure during the healing period, which can be three to seven days.
As with other collagen induction therapies, results are not immediate. “Most patients will see an immediate ‘glow’ on their skin, but results continue to improve for up to six months after the session, as the collagen production that will ease the fine lines and scars continues,” says Dr. Isaacson.
The number of sessions needed varies based on the patient’s concerns and goals. “Patients who have deep wrinkles, stretch marks or acne scars may need six to eight sessions at six-week intervals,” says Dr. Berzin.
Microneedling Indications
“The two top indications for microneeedling in my practice are scars (surgical, acne, traumatic) and general skin rejuvenation, particularly for skin texture and fine wrinkles,” says Dr. Johnson Lee. Additional indications include hyperpigmentation, perioral rhytides, striae and enlarged pores, specifically on the nose.
Jason Emer, MD, a plastic surgeon practicing in Beverly Hills, California, uses microneedling to enhance post-treatment medication delivery, but he finds that the procedure alone takes too long to achieve significant improvement for indications like scars, striae and alopecia; therefore, he prefers to combine it with laser treatments and RF, “which is great for deep tissue heating, tightening and scar remodeling,” he says.
While there is a dearth of clinical evidence to support the effectiveness of microneedling as a treatment for wrinkles and skin rejuvenation, there is some research to support the procedure as a treatment for scars. One of the latest reports comes from the National Institute of Medical Sciences, Jaipur, India, and was published in the Journal of Cosmetic Dermatology (January 2016). The split-face study of 50 patients with atrophic acne scars compared microneedling alone to microneedling combined with PRP. Evaluation with Goodman’s Qualitative Scale showed an excellent response in 40% of the patients and a good response in the remaining 60% when the modalities were combined. The response for microneedling alone was excellent for 5%, good for 84% and poor for 6%.
Another pilot study (Journal of the American Academy of Dermatology, May 2016) evaluated the combination of microneedling and transexamic acid in 32 patients with post-acne erythema, concluding that the combination was “a new and fast treatment for this difficult problem.”
Photo copyright Getty Images.
[pagebreak]
Two other small studies suggested additional indications for microneedling—melasma and infraorbital dark circles. The Brasilian Society of Dermatology’s journal (Brasilian Annals of Dermatology, November/December 2015) included a report of 22 patients with recalcitrant melasma who were treated with two sessions of microneedling 30 days apart. No additional medication was used with the microneedling but patients were instructed to use a lightening treatment daily beginning 24 hours after the microneedling procedure and to apply sunscreen (SPF 60). All of the patients were satisfied with the results of their treatment.
A case study of 13 women with infraorbital dark circles from Athens, Greece (Journal of Cosmetic and Laser Therapy, April 2016), showed significant aesthetic improvement in more than 90% of the patients treated with a combination of microneedling and 10% trichloroacetic acid.
Different Approaches
While basic microneedling procedures don’t vary much from practice to practice, adjunctive therapies do. Some practitioners infuse a variety of topical preparations during and after microneedling; others are very cautious about applying additional medications before or within the first eight hours after the procedure.
“We have found that the MicroPen by itself works, but we believe it works much better in combination with Eclipse Platelet-Rich Plasma. We apply PRP as the lubricant by dripping it upon the selected area before, during and immediately after treatment, then allowing it to set for an hour for enhanced absorption,” says Dr. Garry Lee. “With deep atrophic scars, we find it best to inject Juvéderm to the approximate height of the surrounding skin—before doing microneedling. We believe this is the most effective way to smooth finer surface height variations.”
Dr. Emer rarely uses microneedling alone. “For most indications and skin types we combine microneedling with other treatments to enhance outcomes,” he says. “We typically do a laser procedure, then microneedle while applying a hyaluronic acid serum, PRP, and vitamin C or hydroquinone to the skin, and we often combine microneedling with peels to get better results.”
Dr. Johnson Lee uses “a hyaluronic acid serum as both my lubricant and treatment adjunct for most patients. Those who have significant inflammation can benefit from vitamin C-based serums. Patients with sensitive skin, severe texture irregularities or scarring, as well as those who require limited downtime can be better treated with PRP in conjunction with microneedling,” he says.
Dr. Isaacson performs “biologic PRP by letting blood from the procedure sit on skin for 15 minutes, followed by a hydrating mask with active biologicals to stimulate collagen,” he says. “The day after the procedure we recommend that patients apply a hyaluronic acid serum and topical antioxidant/collagen stimulating lotion that we sell under our office label.”
Dr. Alster is less inclined to combine microneedling with topicals, citing a lack of evidence of efficacy and the possibility of causing dermatitis. “One exception is PRP for hair growth stimulation,” she says, “but even there I tend to use injections of PRP rather than combining it with microneedling.”
Linda W. Lewis is the contributing editor of MedEsthetics.
Photo copyright Getty Images.