New developments in rosacea call for dermatologists to place greater emphasis on addressing persistent facial erythema, according to experts who took part in a recent National Rosacea Society (NRS) roundtable. The goal of the roundtable discussion was to provide an update on this key aspect of the disorder, based on the new standard classification system, recent burden-of-illness study results, new standard management options and significant advances in medical therapy and patient care.
Drawing from current scientific knowledge as well as clinical experience, the new standard classification of rosacea shifted away from subtypes and instead identifies the various phenotypes that may occur in many possible combinations in individual patients, noted Richard Gallo, MD, chairman of dermatology at the University of California, San Diego.
The experts agreed that dermatologists should now consider rosacea as a single disease with multiple potential phenotypes, recognizing persistent facial erythema as the primary diagnostic feature. Phymatous changes, although less common, are also diagnostic, and additional major signs include papules and pustules, flushing, telangiectasia and certain ocular manifestations. The presence of any two of the major phenotypes may be considered diagnostic. Secondary phenotypes include burning, stinging, edema and dryness.
“Rosacea encompasses a multitude of possible combinations of signs and symptoms, and we now have an arsenal of medical therapies to address each of them directly,” Dr. Gallo said. “It is more important than ever that patients are made to understand that effective treatment is more than simply ‘Take your medicine.’ The good news is that a combination of rosacea therapies may often offer a synergistic effect, and a clear and detailed explanation of how exactly to use the various oral and topical therapies can help provide results that will improve quality of life.”
He noted that recent studies have shown that rosacea’s diverse features appear to be part of a consistent continuum of inflammation. As a result, medical therapies that work by reducing inflammation may be useful in treating not only papules and pustules, for instance, but also erythema.
Persistent Redness is Most Damaging to Quality of Life
The NRS has collected data on the social and emotional effects of rosacea and erythema from patient surveys in its newsletter, Rosacea Review. In a survey of 1,675 patients, 82 percent of those who suffered from erythema reported the condition had a negative impact on their general outlook on life, with the figure rising to 90 percent for those with moderate-to-severe redness.
The greater quality of life impact on those with more severe redness was echoed in a recent burden of illness study on facial erythema in rosacea (Baldwin, Dermatologic Therapy, 2019). In the comprehensive survey of 708 respondents, the most common symptoms were flushing lasting longer than 10 minutes (84 percent) and persistent centrofacial erythema (69.1 percent).
“While the patients reported flushing as the most common sign, they named redness as the most bothersome,” said Hilary Baldwin, MD, associate professor of dermatology at Rutgers Robert Wood Johnson Medical School and one of the authors of the study. “And the more severe their facial erythema, the more bothersome it was, even more so than bumps and pimples.”
Julie Harper, MD, president and owner of the Dermatology and Skin Care Center of Birmingham and another author of the study, observed that in spite of its considerable impact on sufferers, physicians often dismiss facial erythema as less serious. “We would never ask psoriasis patients which symptom bothers them most,” she said. “All of a rosacea patient’s symptoms bother them, and we need to treat them the same as psoriasis patients.”
Therapeutic Options
The doctors noted there are few FDA-approved therapies specifically for the erythema of rosacea. Though both are alpha agonists, they act on different receptors and have different actions, said Linda Stein Gold, MD, director of dermatology clinical research at the Henry Ford Health System.
“Brimonidine kicks in within 30 minutes and many patients see a dramatic reduction of their erythema,” said Dr. Stein Gold who noted that exacerbations of redness have also been reported with peaks coming at approximately 3-6 hours and again as the medication began wearing off at 10-12 hours. A possible remedy may be to apply one rather than five pea-sized amounts, which is instructed in the package insert, to various areas of the face.
Oxymetazoline, the other FDA-approved alpha agonist, has a more gentle onset with some improvement evident in 1-3 hours and continued impact seen over the course of the day, while the return of erythema can occur in a more subtle way. The exacerbation of erythema seen with brimonidine was not seen in the oxymetazoline clinical trials, Dr. Stein Gold said. Overall, for many patients, oxymetazoline results in normal-appearing skin tones and may be easier for patients to use, leading to better compliance with therapy.
Though the quality of evidence is limited, light devices including intense pulsed light (IPL) and pulsed dye and potassium titanyl phosphate (KTP) lasers are well established in practice and have been shown to be highly effective in removing telangiectasia and diminishing erythema. A small study comparing IPL and pulsed dye laser found a 60 percent reduction in erythema, versus a 45 percent reduction with pulsed dye. (Tirico Journal of Cosmetic Laser Therapy, 2020.)
While rosacea is still treated by many with a monotherapy approach, the roundtable participants agreed that treating every present phenotype with targeted therapies in cooperation with the patients will achieve the best overall outcome, both objectively in terms of clear skin and subjectively in terms of quality of life.
Patient Education
Dr. Harper noted that it is important to manage the patient’s expectations. “State that clear skin is the goal. If we don’t shoot for it, nobody’s going to make it,” she said. “It’s going to take more than one visit, and you’ll probably have to use more than one tool.”
The initial visit should include five elements, she said: identifying the visible signs of rosacea (including erythema, telangiectasia, papules and pustules, and phymas); ascertaining what bothers the patient (including invisible symptoms such as burning and stinging); discussing trigger factors and how to avoid them; educating about skin care and sun protection; and devising a treatment plan.
“You have this full menu of rosacea—redness, bumps and pimples, ocular symptoms, et cetera,” said Dr. Harper. “It’s like a meal, but just as you can’t eat everything with one utensil, you can’t use just one drug to treat every sign and symptom.”
A combination of medicines aimed at specific phenotypes may work more synergistically overall when taken together than when staggered. Dr. Harper cited a study by Dr. Stein Gold that found using brimonidine for erythema together with ivermectin for papules and pustules from the start resulted in clearer skin than using brimonidine only after several weeks had passed. “If you use just one, you could miss some benefit,” agreed Dr. Stein Gold.
In addition to designing a comprehensive treatment plan, educating the patient on compliance, including time of day and frequency and areas of application should be clearly explained. For example, a patient who applies oxymetazoline before going to bed won’t see the full benefit of treatment.
Ensuring that patients understand the reason for and value of their therapies as well as how properly to use them is part of the physician’s challenge, the doctors noted. “Patients should also be reminded that therapy is intended not just to eliminate existing features, but to maintain remission,” said Dr. Gallo. “With patients I liken it to brushing your teeth—you’re not treating a cavity with toothpaste, you’re preventing future cavities.”
The roundtable was made possible by an educational grant from EPI Health.
For more information, visit www.rosacea.org.
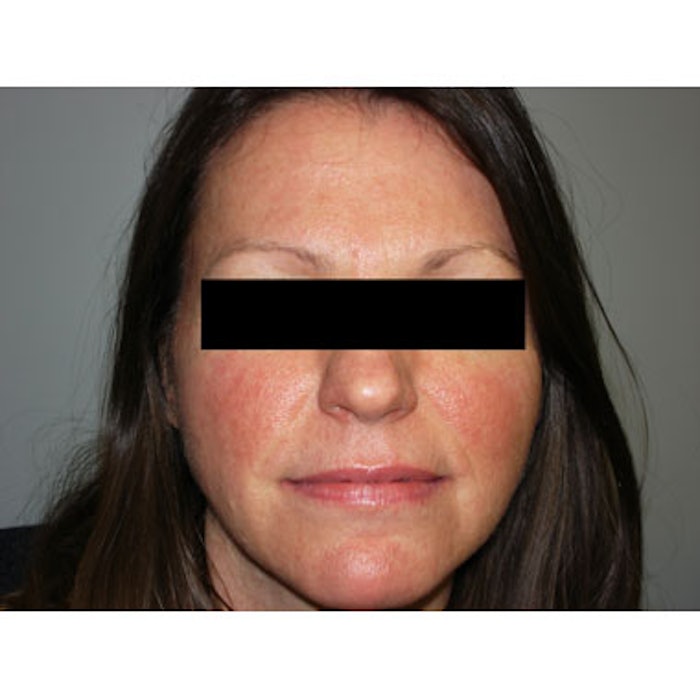
Image: Rosacea patient with facial erythema, courtesy of the National Rosacea Society