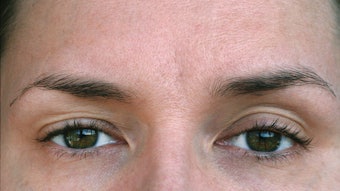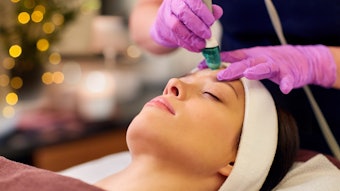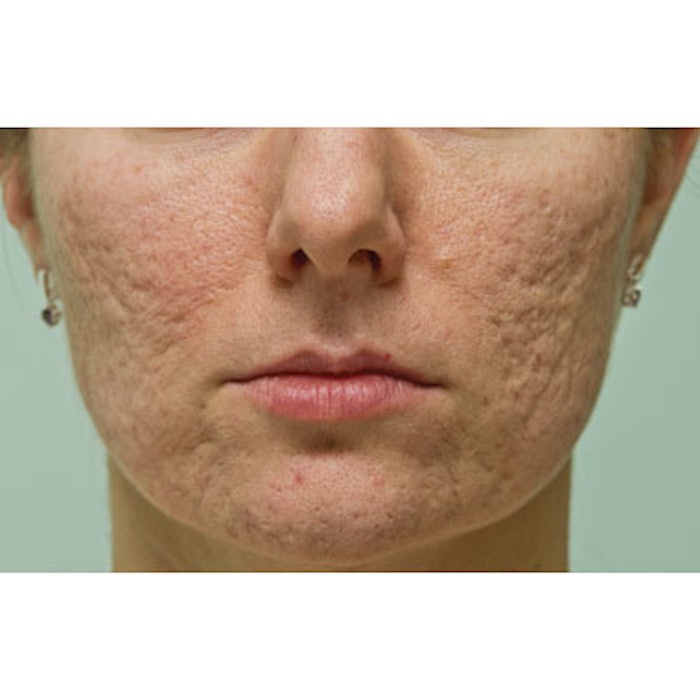
Acne scars affect patients’ self-esteem and self-confidence long after their acne breakouts have cleared. The frustration for practitioners and patients alike is that there have traditionally been few effective treatments to eradicate the deep scars of acne. While there remains no single treatment modality that can completely erase the textural and pigmentary changes experienced by patients, physicians are achieving improved outcomes through the use of lasers, peels and fillers in combination with more invasive options, like subcision and punch grafts.
“Acne and acne scarring are extremely emotional conditions,” says Vic Narurkar, MD, director and founder of the Bay Area Laser Institute in San Francisco. “While I do many things in my practice, the happiest patients are the ones for whom we improved their acne scarring. It is life changing.”
One of the most challenging aspects of acne scar treatment is that there is no one-size-fits-all solution. Since scars come in multiple forms—rolling, boxcar, ice pick and pigmented— physicians must create a customized regimen that best matches the individual patient’s needs, says Ruth Tedaldi, MD, founding partner of Dermatology Partners in Wellesley, Massachusetts.
The key to achieving high patient satisfaction is to set realistic expectations and avoid over-promising and underdelivering. “Patients should not expect removal of the acne scar, but improvement in the appearance of the scar,” says Dr. Tedaldi. “With today’s treatments, the topography of the skin becomes much less angulated and simple camouflage with makeup becomes easier.”
The topographic depressions of acne scars are the result of compromised collagen production, formed during the natural wound healing process. The perpendicular bundles of collagen created during active acne breakouts anchor the skin of the scars down.
“The majority of patients have atrophic or ice-pick scars,” says Jill S. Waibel, MD, a dermatologist at Miami Dermatology & Laser Institute. “Both of these types of scars result from loss of collagen deposition during the wound healing process of acneiform lesions.”
Superficial approaches, used to increase collagen production and tighten skin, include glycolic acid chemical peels as well as topical tretinoin and topical hydroquinone for skin surface improvement and pigmentary variation. But these approaches have limited success, says Dr. Waibel.
Laser Skin Resurfacing
Fractional lasers—both ablative and nonablative—have built on the limited success of chemical peels. Both devices are used to stimulate collagen production, which helps to replace scar tissue with more normal collagen, and tighten the skin to reduce the depth of acne scars.
Murad Alam, MD, professor and director of cosmetic dermatology at Northwestern University in Chicago, prefers nonablative fractional resurfacing. He admits his practice is conservative when it comes to laser resurfacing: Densities and energy levels are gradually increased, and at least six treatments are usually delivered over a comparable number of months.
“You have to make sure the aggressiveness of the procedure is coincident with the patient’s lifestyle,” he says. “In general, it is easier for people to hide out for several individual weekends, as with nonablative devices, than for two weeks continuously, as with ablation.”
Photo copyright Getty Images.
[pagebreak]
During the consultation Dr. Alam explains to patients who have darker skin that they may need more than the usual number of treatments delivered at lower energy levels to avoid post-inflammatory hyperpigmentation.
Nonablative laser procedures are less expensive and easier for patients to tolerate in terms of both pain and downtime, but they may not be as effective as ablative treatments and typically require several treatments, says Suzanne L. Kilmer, MD, founding director of the Laser and Skin Surgery Center of Northern California and clinical professor at the University of California, Davis.
To improve acne scars, she uses a fractional ablative laser that can penetrate deep into the dermis to reach the scar tissue at low density settings to minimize downtime. “They can make smaller holes and go deeper, as much as 6mm, so your patient can get more improvement yet still heal faster,” Dr. Kilmer says. “If you ablate the tissue, you remove scar tissue in the affected area and it heals from the inside. It hurts more and creates a wound, which means your patient will have to do wound care and soaks.”
However, the downtime is not necessarily longer. “A nonablative fractional laser treatment causes the skin to look pink and swollen for a few days. With an ablative treatment, they’ll be bloody for a few days,” says Dr. Kilmer. She notes that higher-powered ablative devices offer benefits: They can deliver the energy with less heat and ablate more efficiently, which reduces the pain during treatment. They are also more effective for thicker scars.
Dr. Narurkar favors fractional laser resurfacing for all types of scars: rolling, boxcar and ice pick. His first line of treatment is the Fraxel Restore Laser, a nonablative, fractional resurfacing laser that uses a 1550nm wavelength. “We’re able to treat all skin types regardless of their pigmentation,” he says. “The laser resurfaces the skin from the inside out and rebuilds your collagen over time so you see an improvement in acne scars.”
While Dr. Narurkar has both nonablative and ablative fractional laser systems, he finds the nonablative unit to be more efficacious for a broader range of patients. “You need to go deep and be able to treat a variety of skin types,” he says. “With an ablative fractional laser, you’re limited in the types of skin pigmentation you can treat. You can be more aggressive with a nonablative unit on darker skin tones.”
He begins his laser treatments at 40mJ, but can increase the energy level to 70mJ, if necessary. Treatment density depends on the patient’s skin type. For a darker-skinned patient, he may do Level 4, which treats less than 20% of the skin. In lighter-skinned patients, he may go up to Level 9, which offers between 30% and 40% coverage.
“Over time, we figured out how to best tailor the procedures to the patient, and we can customize the treatment density and the energy levels with the Fraxel based on what we are treating,” says Dr. Narurkar. “A patient may come in with deeper acne scars in certain areas and more superficial scars in others. We can adjust the intensity of the energy as well as treatment density to truly give them a customized treatment. Nothing else allows you to do that in a consistent fashion.”
Filling Scars
If fractional lasers and peels are not sufficient, physicians can elevate rolling scars by injecting dermal fillers into the valleys. Dr. Tedaldi uses Bellafill (polymethylmethacrylate microspheres and collagen, Suneva Medical), the only dermal filler currently approved by the FDA for the treatment of moderate to severe, atrophic, distensible facial acne scars on the cheek.
“My acne scar patients have been pleased with the level of correction achieved with Bellafill, and I’ve found that the filler is effective for both new and old scars in many age ranges, 21 and up,” she says, noting that active acne breakouts must be controlled prior to injection with Bellafill.
Photo copyright Getty Images.
[pagebreak]
Hyaluronic acid fillers are also used off-label to fill scars and even out skin texture. “Indeed, despite the conventional wisdom, a hyaluronic acid filler can be injected even into fine ice-pick scars, superficially, in minute aliquots of 0.01,” says Dr. Alam. He adds that injectors must use caution to avoid bluish discoloration at the area of injection.
Since filler injection results are temporary—Bellafill is a semipermanent filler, but may require multiple injections to reach the desired volume—patients may need to repeat the injections periodically, cautions Dr. Kilmer. “Also, if you are not careful you can create a doughnut effect where the filler fills around the scar and the scar is tethered down. These are nice ways to treat scars, but they are temporary,” she says.
Subcision and Punch Grafts
Rolling scars also respond well to subcision with a Nokor or similar needle, which is safe even in patients with darker skin types, says Dr. Alam. Patients with deep ice-pick acne scars are good candidates for excision and punch replacement grafts. In excision, cuts are made into the skin to remove the scar tissue and then the wound is closed with stitches. With punch replacement grafts, a round sharp tool—matched to the size of the scar—is used to remove the scar tissue. A skin graft is then used to fill the wound.
“Sometimes these treatments can be combined with laser resurfacing for maximized results,” says Dr. Tedaldi. “Skin tightening—which utilizes radiofrequency to tighten the skin—is also an option.”
Dr. Alam recommends punch elevation particularly for deep, large boxcar scars. Punch elevation is similar to punch grafting, but the tissue is not extracted. Rather, the punch pulls the tissue up and it is then sutured flush to the surrounding epidermis.
For smaller boxcar scars, Dr. Alam uses chemical reconstruction of skin scars (CROSS), a technique which uses high concentrations of trichloroacetic acid (TCA) in a pinpoint fashion. TCA is applied directly into each scar to stimulate collagen production. Ultimately, it causes the scar to rise up, flatten and close. One benefit is that the recovery time is limited to only the treated areas. “Ice-pick scars may also respond to CROSS, but it should be avoided in darker skin which tends to hyperpigment,” he says.
Once textural changes have been addressed, Dr. Alam treats residual erythema with vascular lasers or intense pulsed light. “If hyperpigmentation has occurred, it will resolve slowly and spontaneously; the physician should distinguish these brown spots from depressed acne scars, and treat them gently if at all,” he says.
Organizing Treatments
Currently, there is no standard dictating the order in which procedures must be performed when multiple modalities are utilized. “The patient’s particular concerns and physical exam dictate order,” says Dr. Tedaldi. “In general, the cardinal rule is to avoid laser in the periprocedural period, within two to three weeks after or before injectables are being used. But there are always exceptions to this recommendation.”
The reality is that for acne scars, whatever modality you use, it is a process, says Dr. Narurkar. It requires not only multiple treatments, but multiple treatment modalities. Sometimes for bound down or tethered scars, in addition to using the Fraxel Laser, Dr. Narurkar will perform a subcision with a Trocar needle to break up the scars. However, he notes this is only for very deep scars.
“Once the scars are improved, and for any that are distensible and atrophic, we then use dermal fillers,” he says. “My preference is the hyaluronic acid-based fillers, such as Juvéderm and Restylane. The reason is that these fillers are reversible, so if for some reason there is a problem, you can adjust them or take it away with hyaluronidase.”
Photo copyright Getty Images.
[pagebreak]
For Dr. Alam, any cutting, whether elliptical excision, punch excision or punch float/elevation, is performed first. Then come less invasive methods to soften the scars, like subcision and CROSS. “Towards the end, you may want to consider fractional nonablative or ablative resurfacing, which hides lines and marks from previous interventions,” he says. “Use of fillers and tightening devices is appropriate at any time.”
Acne scar treatments are most effective when delivered after active acne breakouts have subsided. “They cannot have uncontrolled acne,” says Dr. Narurkar. “At any given time, you will have patients who have occasional breakouts. We manage the actual acne first, so it’s under control before we start scar treatments.”
Getting a handle on active acne is also the first step in preventing or reducing long-term acne scarring. “Patients more prone to scarring have increased cytokines and growth factors,” says Dr. Waibel. “Treating the active acne lesions with laser can decrease inflammation, and the fractional laser may be able to alter the inflammatory cascade which may, in turn, prevent scarring. Our colleagues in China have done studies looking at laser treatment of patients on isotretinoin and have shown decreased scarring in this cohort.”
What the Future Holds
The significant emotional toll of acne scarring combined with the lack of a gold standard of care for these patients has kept acne scar research in the forefront of dermatology.
In June 2014, Dr. Waibel and her colleagues published a paper in Dermatologic Surgery on laser-assisted delivery of topically applied Sculptra (poly-L-lactic acid, Galderma) for the treatment of atrophic scars, including acne scars. Scupltra, an injectable filler, is typically injected into the subcutaneous or supraperiosteal plane to correct facial volume.
“Once implanted, the material stimulates fibroblast proliferation and neocollagenesis,” says Dr. Waibel. “The study evaluated the poly-L-lactic acid with the properties of a fractional ablative laser to improve atrophic scars. This combination takes advantage of both of their inherent properties in up-regulating new collagen synthesis to improve atrophic scars.”
In addition, Dr. Waibel is working with an Acelity product called Cellutome for epidermal grafting. “This novel device, currently used to perform epidermal grafting procedures, is a donor site-sparing harvesting system which enables the transfer of autologous epidermis that includes live melanocytes,” she explains. “This epidermal harvesting system technology creates micro-suction blisters, known as microdomes, by using a combination of vacuum and warmth. It allows for epidermal skin grafting in the outpatient setting with less risk of donor site morbidities like scarring.”
Although options for acne scar treatment are improving, prevention remains the best practice for patient care. “The best policy for dermatologists is to get to the patient early and control their inflammatory and cystic acne prior to scar development,” says Dr. Waibel.
Daniel Casciato is a Pittsburgh-based freelance writer.
Photo copyright Getty Images.