Cancer treatments and surgery also wreak havoc with the patient’s appearance in other ways—causing eyelashes and brows to fly off the face, making hair fall out, leaving scars in the place of breasts.
Aesthetic services, ranging from skincare and hair restoration treatments to permanent makeup services, can give back what surgery, chemotherapy, and radiation take away. “The hospital and medical staff does a great job treating cancer, but I am there for [the patient’s] body image issues, the emotional issues,” says licensed esthetician Becky Kuehn, who is certified in Oncology Esthetics. Kuehn works with cancer patients at two hospital-based cancer centers in Washington State.
“Each person uniquely experiences the cancer ‘journey,’” says Kuehn, a cancer survivor herself. “I had hair loss, skin issues, and horrible mouth and GI issues from chemo. This gave me an understanding of what my clients might be going through—how chemotherapy affects the whole person, as well as the emotional and psycho-social side effects.”
As the U.S. Director and National Educator for Oncology Esthetics, Kuehn trains other estheticians, “so they will never turn away a client, especially a client that needs them the most,” she says.
While providing oncology aesthetic services is truly a do-good, feel-good endeavor, those who dip their toe in the specialty will have no dearth of patients. Cancer patients comprise a large and growing group.
In the United States, women have a 38% risk of developing cancer. For men, the odds are even worse: Nearly 44% will be diagnosed with cancer in their lifetimes. “Cancer is common, and many forms of cancer are chronic diseases people live with for years,” says Dr. Bailey. “The number of cancer patients seeking aesthetic products and treatments is only going to rise.”
Topicals and Peels
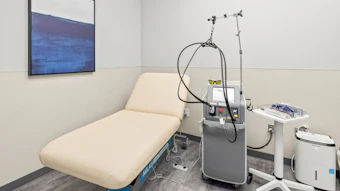
“Skin is the most visible organ system to suffer during cancer treatment, and the right skin care can provide great comfort. It’s bad enough to have cancer and endure treatment, so it’s nice to control some aspect of your appearance during such an out-of-control time,” says Dr. Bailey.
Image copyright istockphoto.com
[pagebreak]
Practitioners need to use extreme care when offering esthetic services to these patients due to the increased risk of infection and photosensitivity caused by radiation and chemotherapy drugs. “When considering esthetic treatments in the setting of an oncology patient, it is imperative to take the approach of ‘first do no harm,’” says dermatologist Cheryl Lee Eberting, MD, director of Alpine Dermatology in Alpine, Utah and founder of the Cheryl Lee MD Sensitive Skin Care Line (cherylleemd.com). “One must consider the major vulnerabilities of the patient. These patients are immunologically compromised, often more likely to have a photo-reaction due to chemotherapy, and may also be undergoing some sort of hormonal manipulation.”
She counsels physicians and estheticians to avoid known hormone disruptors, like soy-based products. “It is not safe to use any photosensitizing products such as tretinoin, retinol, alpha-hydroxy acids, and many plant-based products, which may be more likely to induce phytophoto dermatitis,” she says.
Dr. Eberting also counsels her oncology patients against the use of supplements, oils or topicals that have any sort of immunomodulatory function. “The immune system of a cancer patient is in a delicate balance during all phases of treatment, and the use of immune ‘boosters’ could be detrimental and could possibly interfere with effective treatment,” she says. “For example, any actives that claim to ‘stimulate the immune system’ (like echinacea) should be avoided during cancer therapy.”
When selecting treatments, Dr. Eberting avoids any resurfacing procedures that penetrate or remove any portion of the epidermis and/or photoprotective layers of the skin, including microdermabrasion, chemical peels, microneedling and fractional resurfacing. “In the postprocedure state, the skin will be particularly susceptible to pigmentary alteration, photosensitization and infection,” she says.
Dr. Bailey does offer facials, gentle microdermabrasion, and mild chemical peels to cancer patients, “all done with extreme care,” she says. “A small wound or superficial infection can rapidly become a crisis on immunocompromised skin. So we use the same disinfecting practices in our esthetics room that we use in our medical treatment and surgery rooms. Also, I have trained my estheticians to understand the skin sensitivity and fragility that occurs during cancer treatment, and how to customize services to safely help these clients.”
Her focus on safety extends to the smallest detail, such as the water used in facial steamers. “If tap water is used, there is mineral buildup on the coils. That becomes a place for germs to proliferate, posing an infection risk to an immunocompromised person” she says.
[pagebreak]
While she was on chemotherapy, Dr. Bailey realized that cancer patients would benefit from a simple, turnkey skincare routine. So she created a Chemotherapy Skincare Kit (drbaileyskincare.com), packed with gentle, hypoallergenic, but highly therapeutic products for cleansing, hydrating, and nurturing the face, hands, and body.
“I want to help cancer patients feel as pretty as possible,” she says. “So [for my patients who have cancer] I create a long-term plan that encompasses the phases of their cancer treatment; I get permission from their medical oncology physician; and I move forward with [dermatological] treatments when they become safe.”
Dr. Eberting also urges practitioners to communicate with both patients and their oncologists when developing an esthetic treatment plan, particularly when it comes to medical treatments, such as lasers, neurotoxins and dermal fillers.
Injectables and Energy-Based Devices
“If the immune system has been manipulated in any way—stimulated or suppressed—there is a very high inherent risk of an allergic reaction or infection, respectively,” says Dr. Eberting. “Fillers penetrate what is left of the body’s defense system—the skin barrier—and introduce foreign material into the skin that may trigger unusual or unintended reactions. Neurotoxins do not deposit foreign material per se, but the skin barrier is broken, so disinfect the skin very, very well if you intend to use them.”
Both doctors agree that lasers pose several problems for patients currently undergoing treatment. “Any sort of resurfacing treatment should be avoided,” says Dr. Eberting. “The skin barrier is broken and infection can and will set in. As for non-resurfacing treatments like laser hair removal, IPL or Nd:YAG, there is a risk of photosensitivity reactions to any number of wavelengths of light.”
Patients who are on a chemotherapy drug called methotrexate or one of the Taxanes, can experience a “photo-recall” reaction three to five days after UV exposure. “The patient will look like they have been sunburned severely without having gone in the sun,” says Dr. Eberting. “The drugs themselves are often photosensitizers, so it is best to avoid any light-based treatments when one is undergoing cancer treatment. If only undergoing radiation therapy without any form of chemotherapy, the risk is less, but still present.”
Dr. Bailey recommends that patients on chemotherapy avoid injectable or laser treatments. But for those who are highly motivated to proceed, she will consider offering IPL, Botox, or fillers on a case-by-case basis, but only after consulting the patient’s oncology team. “A conversation with the medical oncologist is essential,” she says. “For injectable treatments I want a patient’s blood clotting function to be fairly normal to prevent excessive bruising. For IPL, I prefer they not be on light-sensitizing medicines. With ablative laser procedures, I want the immune system to be relatively normal.”
[pagebreak]
Ruby Powell, an oncology-certified licensed esthetician in Fort Worth, Texas, also checks with the patient’s oncologist before providing treatment to these patients. “I require the oncologist’s approval through a Physician Release. You always want the oncologist to know what is happening in their patient’s life.”
Powell customizes her treatment protocols and product recommendations for cancer patients. “I use the Lindi Skin line (lindiskin.com), which is designed to combat the harsh effects of cancer treatment and help soothe and heal,” she says. “My techniques are also different for cancer patients: no steamer, no hot towels, no brush during cleansing, limited essential oils and customized massage techniques.”
Powell considers education part of her service. “Patients need to learn how to care for their skin,” she says. “They need to know what conditions and reactions should be brought to their oncologist’s attention. They need to know which ingredients are safe. Post-treatment, they may be allergic to ingredients they weren’t allergic to in the past.”
Crowning Glory
When a woman learns she will be treated for cancer, her first question will often be: “Will I lose my hair?” Though others (including her family, friends, and even her oncologist) may dismiss her concerns as being superficial, she naturally fears the loss not only of her looks, but of her identify.
In most cases, hair eventually grows back. But not always. “Many patients who had [cancer] treatment lose hair permanently. Hair loss becomes a public, visual reminder of their disease,” says Connecticut cosmetic surgeon Scott A. Boden, MD, a board certified hair transplant surgeon with expertise in hair loss due to radiation therapy.
“[Hair restoration] for patients who have survived cancer extends beyond a purely elective cosmetic procedure — it can be life-affirming,” says Dr. Boden, who has performed about 3,000 hair transplant procedures.
He shared a recent experience with a breast cancer survivor: After her doctor told her that she would need a mastectomy, she was referred to a reconstructive surgeon to discuss breast restoration. The patient later told Dr. Boden, “I wish they [had instead] brought me to your office! I can wear a breast prosthesis and nobody sees that I have had cancer. But when I lost my hair and it didn’t come back, that was the most painful part of going out in public. Getting my hair back is what enabled me to be myself again.”
Managing patient expectations is critical. “A second procedure to increase the density of the transplanted hair may be required,” he says. “And physicians need to somewhat modify their techniques to successfully transplant into scarred areas.”
[pagebreak]
Replacing What Was Lost
Permanent makeup services play a vital role in helping patients return (aesthetically) to their pre-cancer treatment selves. Nipple areolas can be recreated as the final step in breast reconstruction. Natural-looking eyebrow tattoos replicate what was lost during chemotherapy. Permanent eyeliner can define eyes, despite thinning or missing lashes.
Master esthetician Ruth Swissa, a permanent makeup artist, creates three-dimensional areolas. She uses organic, custom-blended, flesh-colored medical micropigments, consisting of tiny droplets of color deposited into the skin’s dermal layer. She also creates permanent, natural-looking strokes that replicate eyebrows lost during chemotherapy and permanent eyeliner to enhance the appearance of the eyes when lashes thin or fall out.
“For breast cancer patients, I charge only for supplies—I do not charge for my time,” says Swissa, who owns skincare spas and permanent makeup studios in Beverly Hills and Agoura Hills, California. For those not ready to commit to permanent pigmentation, Swissa also creates temporary realistic-looking 3-D areola tattoos, available in several colors and sizes.
With such a robust need for oncology aesthetic services, providers say they don’t have to market their services. In most cases, they receive patients by referral. Oncologists and other members of the patient’s healthcare team—and even other providers, such as wigmakers—often send patients their way.
Jeanine McTasney, a certified permanent cosmetic professional and fellow of the American Academy of Micropigmentation, receives the majority of her patient referrals from Breastlink, a freestanding breast cancer center in Orange, California. “Breastlink schedules the tattoo, and I complete it in their facility,” she says. “Most often one of the physicians appears during the procedure to check on the patient.”
To help physicians and patients find a qualified tattoo technician, McTasney founded the National Areola and Nipple Tattoo Registry (nationalareolanippletattooregistry.com). “I also developed the registry to assist technicians in training on tattooing techniques and education on insurance billing,” she says. Training is also available through companies, such as the Nouveau Contour Academy (nc-academy.com).
Aesthetic dermatologic services go a long way toward helping cancer patients look and feel “normal,” Dr. Bailey says. “As both an oncology patient and the owner of aesthetic service businesses, I have made it my job to meet the needs of people like myself.”
Maryann Hammers is a freelance writer, specializing in the medical, beauty and spa industries.