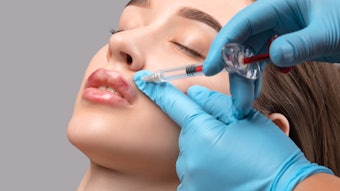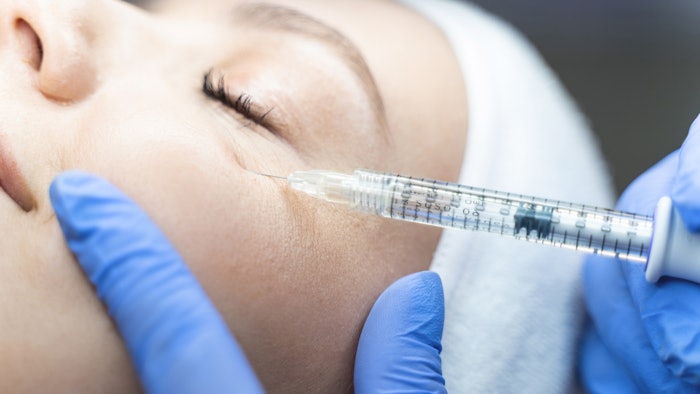
An interdisciplinary panel of aesthetic physicians has developed consensus guidelines on the use of hyaluronic acid (HA) fillers for the treatment of tear troughs. Published in the Journal of Cosmetic Dermatology (January 2021), the guidelines cover patient selection, anatomical considerations, injection technique and filler selection.
The authors note that in order to safely and properly correct tear trough deformity with HA injection, injectors must have good anatomical knowledge of the area and involvement of the structures in the tear trough, carry out proper clinical assessment of the patient, choose the correct product and use an appropriate injection technique.
Related: Undereye Concerns
Candidates for the procedure include those with excess fat in inferior palpebral fat pads with septal laxity, receding of the inferior bony orbital rim, hyperprojection of the intrinsic suborbicularis oculi fat (SOOF) caused by displacement of tissue with age or due to excess malar fat volume or muscle thickness defect (displacement of neighboring tissues) and thickness defect of skin or subcutaneous muscle tissue.
When it comes to product selection, HA fillers with a high level of cross‐linking are longer lasting, but also increases water absorption and subsequent edema and may produce more adverse reactions. Therefore, the guidelines recommend use of fillers with less cross-linking and less water rentention.
Injections, whether the injector is using a needle or cannula, must be deep to avoid compression in the lymphatics and to avoid the appearance of the Tyndall effect. The panel does not recommend the injection of the mini‐fat pad that exists in some patients, between the orbitomalar and zygomatic‐malar ligaments, due to the potential risk of altering lymphatic drainage, nor injection at the level of the orbitomalar ligament or cranially to it.
Injections must be slow to allow the product to accommodate properly to the depression and to avoid overcorrection. Unnecessary movements of the cannula or needle must be avoided to prevent or reduce trauma to the tissues and, in particular, to the delicate lymph vessels.
They recommend a maximum of 0.5 ml of filler per tear trough and session, noting that “It is advisable to initially perform undercorrection, as the HA injected will undergo a process of consolidation, drying and subsequent rehydration in the next 30 days. More HA may be added in subsequent sessions considering this time frame.”
Read the full guidelines here.