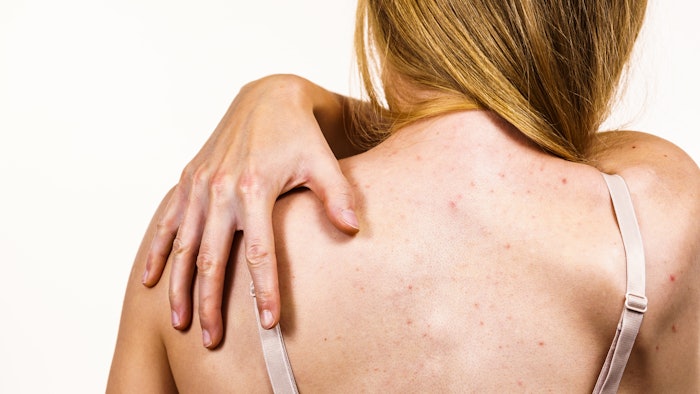
Fungal acne is a type of infection in the skin’s hair follicles that commonly appears as small pimples that don’t vary much in shape or size. Fungal acne can cause whiteheads and skin irritation and is often confused for acne vulgaris. It is diagnosed by a dermatologist based on appearance and symptoms and is typically treated with a topical cream or shampoo.
Related: Using BoNT-A to Temporarily Treat Acne Vulgaris
Per Healthline, fungal acne often shows up on the arm, chest and back. It is caused by an overgrowth of yeast that is always present on the skin. If the natural balance of the skin is altered, the infection of hair follicles develops and acne-like symptoms will appear on the skin. Sweat clogging the hair follicles, excess oil production, and shaving, waxing or plucking hairs are a few factors that could lead to the development of fungal acne.
The pimples caused by fungal acne tend to show up in clusters and all be the same size, which differentiates it from bacterial acne, which typically has variable-sized pimples. Fungal acne also causes itchiness, which is rare in bacterial acne.
To prevent fungal acne, it is recommended for at-risk patients to shower after sweating, wear looser clothes, eat a balanced diet and use a dandruff shampoo as an off-label body wash.
Topical treatments are the standard for fungal acne. Some of the most common treatments are selenium sulfide shampoo, 2% ketoconazole shampoo, ketoconazole cream, econazole cream and solution propylene glycol cream. Patients may also benefit from oral antifungal medications, either over the counter or prescribed.
Researchers have looked at alternatives to improve the application of topical creams to treat skin conditions, including fungal acne. Some of the standard anti-infective drugs can be limited by poor water solubility, low bioavailability and poor targeting efficiency, which can lead to poor efficacy, adverse effects and drug resistance.
A January 2023 study found that hydrogel-based therapies can be used as drug carriers for the treatment of infectious skin diseases and as auxiliary methods for the alleviation of pain during the treatment process. Hydrogels are used with good efficacy for skin wound healing, but their clinical applications in the treatment of skin infections are less frequent.