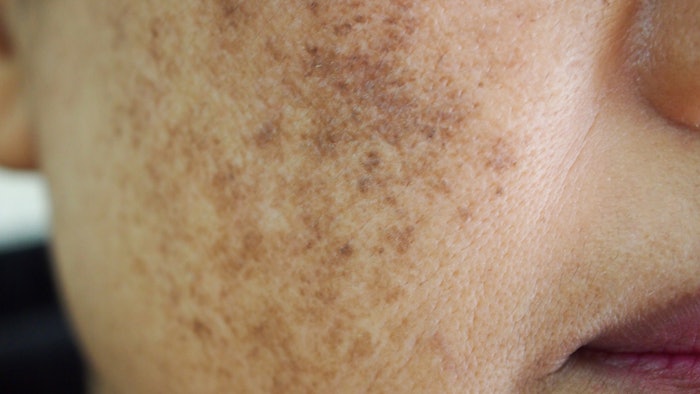
While the sunny summer weather is a welcome respite to the long year we have all had, it also is a season that is difficult for patients struggling with melasma. The heat combined with more time outdoors often leads to the first time appearance of melasma or a worsening of symptoms among those already in treatment.
At the Face & Body with MedEsthetics virtual event on May 25, dermatologist Mona Sadeghpour, MD, founder of the SkinMed Institute in Lone Tree, Colorado, presented “Stepping out of the Shadow: An Evidence-Based Approach to the Diagnosis and Management of Melasma.”
Diagnosis
Melasma is the result of the body producing more pigment than it is able to eliminate, due to overactive melanocytes and, in some cases, increased vasculature. But not all dark spots are melasma, Dr. Sadeghpour noted.
Melasma presents in one of three distinct patterns of hyperpigmentation: centrofacial, which involves the mid face, forehead and upper lip (most common); malar pattern; or mandibular pattern (least common).
If the patient has skin inflammation, this gears you away from melasma. “Melasma is not typically associated with inflammation; this may be another skin disorder,” said Dr. Sadeghpur.
Related: Most Common Pigmentation Concerns in Skin of Color
For patients without inflammation and a familiar pattern of melasma, obtain a good medical and family history. A positive family history increases risk of treatment resistance.
Use a Wood’s lamp to determine placement of pigment. The Wood’s lamp will enhance epidermal melasma; it does not enhance dermal melasma. Deeper dermal pigment will look a little lighter (lighter brown or bluish with poorly circumscribed borders). Epidermal pigment is darker with well circumscribed borders.
“The Wood’s lamp is not perfect, but it does give you a rough estimate of what you may be looking at, which can guide your treatment.” said Dr. Sadeghpour.
She also uses dermoscopy to look at vasculature in the area of the pigmentation. “If there is more vasculature within the lesion, pulsed dye laser may be a modality to consider down the line. But this is not a first line treatment,” she noted.
First Line Treatment
Always start with topical therapy and strict sun protection. This is the gold standard therapy. First line treatment is hydroquinone (HQ) 4% twice daily—“It’s important to use it twice daily, not once daily,” noted Dr. Sadeghpour—plus sun protection. She recommends a tinted sunscreen that includes iron oxides that block visible light, which can worsen melasma, especially in patients with skin of color.
Retinoids (tretinoin .5% or 1%) in combination with sun protection are also a “wonderful choice,” she said. For pregnant patients who cannot use HQ or retinoids, she recommends topical azelaic acid 20% twice daily.
Triple combination creams, such as Tri-Luma, which contain HQ, retinoids and steroids have been shown to be effective, but she does not use them as first-line therapy as exposure to the tretinoin can cause enough irritation to create PIH. In addition, steroids can induce acne in patients prone to acne. Therefore, she prescribes them only for patients who fail HQ 4%.
“Be really careful with triple combination, especially for people who have sensitive skin,” she noted.
You also want to identify risk factors and mitigate them, when possible. Risk factors for melasma include:
- Fitzpatrick Skin type III-IV
- Exposure to UV radiation
- Exposure to visible light, especially in skin of color patients
- Family history of melasma
- Pregnancy
- Exogenous hormones (oral contraceptives and hormone replacement therapy)
- Heat, which causes vasodilation and inflammation that can exacerbate melasma
- Endocrine disorders (thyroid, adrenals, etc.)
If the patient is on an oral contraceptive, ask them to switch to a different contraceptive with less hormonal exposure, if possible.
Help patients minimize as many triggers as you can. This includes educating patients on strict photoprotection and sun avoidance.
If the patient is exposed to heat either through the outdoors or their work (hair dryers, ovens, etc.) they can use a handheld fan or a cool towel to decrease the heat on their skin when they feel their faces getting hot.
Second and Third Line Treatments
If a patient does not see significant improvement in three to four months with topical therapies, consider oral tranexamic acid, peels or lasers in combination with topical therapy and sun protection.
Dr. Sadeghpour prescribes oral tranexamic acid (TA) for patients who have failed topical therapies, as well as for patients who have “really deep” dermal pigment. “I have patients take one 650 mg tablet once a day,” she said. “It will take a few weeks to see improvement, and there is a chance of relapse after they stop taking it.”
Related: Oral Tranexamic Acid Helps Prevent PIH
Patients must be screened for thromboembolic disorder as well as family history of stroke or heart disease before using oral TA. Also ask if they are on an oral contraceptive, which may increase risk for blood clots.
Lasers and peels are never first line treatments. However, they can be used in conjunction with topicals for patient who have maxed out with topical therapies.
Glycolic acid has the most evidence for use in melasma. “But it has never been studied head-to-head with topicals,” said Dr. Sadeghpour. “I never use peels in my practice because they can cause irritation and make melasma worse. But in the hands of an experienced peeler, glycolic acid can help with melasma.”
She starts her patients with topical therapy and evaluates them after three to four months. “If we’ve maxed out with topicals, then I look at laser using slow and steady, non-aggressive, low-energy and low-density treatments,” she said.
There are only three lasers that have a high level of evidence for melasma: Q-switched 1,064nm Nd:YAG (low energy/low fluence); 1,927nm low energy/low density (Clear+Brilliant Permea); and Picosecond 1,064nm. “You never use lasers alone without adequate topical therapy and sun protection,” said Dr. Sadeghpour, who pretreats her patients for a month with HQ, azelaic acid or Retin-A before laser treatment.
Related: Zapping Away Pigment
“Laser treatments will require maintenance treatments, which is costly and may not be feasible for the patient,” she added.
The key takeaway for patients and practitioners is that melasma is a chronic condition. “There is no way to cure it, we can only hope to control it,” said Dr. Sadeghpour. “I tell patients, ‘You have hyperactive pigment-producing cells that are constantly in overdrive, and we need to work together to put these hyperactive kids to sleep so they don’t cause as much trouble.’”