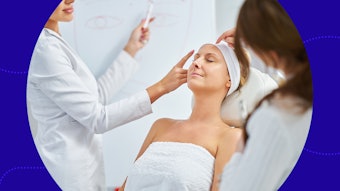
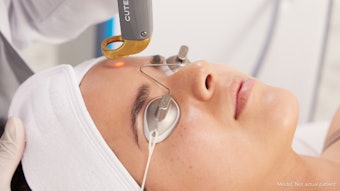
Since it first received U.S. Food and Drug Administration (FDA) approval in 1995, intense pulsed light (IPL) has become one of the most versatile and widely used technologies in aesthetic medicine. It has been used for permanent hair reduction and to treat a variety of concerns, including redness, acne and excess pigmentation. Now that it has been joined by a number of lasers and energy-based devices, the question for providers is: Which patients and indications benefit most from IPL?
Top IPL Indications
Photorejuvenation in fair skin. “IPL is still the No. 1 treatment for global skin rejuvenation and photodamage because it covers vascular concerns, pigmentation problems and stimulates collagen production,” says Michael Gold, MD, of the Gold Skin Care Center in Nashville. “If you have a patient who has predominantly photoaged skin with some wrinkling, some red spots and some brown spots, there is no other device that will treat all those concerns simultaneously.”
Mary Lupo, MD, of the Lupo Center for Aesthetic & General Dermatology in New Orleans, agrees that “IPL is sort of a shotgun treatment in that you can address both redness and brown pigment with one device. With lasers, these would have to be treated separately. So IPL is more of a generalist than a specialist device.” But she cautions that there are limitations. “It is very important to look at the patient’s skin type,” she says. “IPL is optimal for skin types I and II. It can be used on skin type III, but the 1064nm laser is safer in darker skin types and more effective for deeper vasculature.”
While IPL is best known for its ability to improve the complexion by targeting redness and pigmentation, there is a growing body of evidence that it can stimulate collagen production and prevent fine lines and wrinkles as well.
In 2012, Stanford University published a study in the Journal of Investigative Dermatology that concluded that treatment with Sciton’s BBL (broadband light) device can change the expression of genes associated with the aging process to more closely resemble young skin. In May 2016, Dr. Gold published the outcomes of more than 2,500 long-term IPL patients in the Journal of Cosmetic and Laser Therapy. All subjects received multiple IPL treatments—the majority underwent annual treatments—for 7 to 12 years. “The results were astounding,” says Dr. Gold. “Some of these patients were 45 at the beginning and 10 years later, they looked younger than when they started.”
“Due to the heat that is generated, IPL does offer some collagen stimulation—and the manifestation of that will be some temporary pore reduction, some overall skin plumping and a reduction in fine lines,” says Dr. Lupo, who notes that although IPL can help maintain skin health and prevent signs of aging, “there is no place for IPL in the treatment of skin sagging or deep wrinkles. This requires a skin-tightening treatment—IPL is primarily a color device.”
Rosacea/vascular concerns. Thanks to its ability to target redness, IPL is widely used to treat the diffuse redness and broken vessels of rosacea. In 2014, Mitchel P. Goldman, MD, co-authored a literature review to provide evidence-based recommendations for the application of IPL. For “Application of Intense Pulsed Light in the Treatment of Dermatologic Disease: A Systemic Review,” (Dermatologic Surgery), the authors searched CENTRAL, EMBASE and MEDLINE databases—dates ranging from 1974 to 2013—for studies that examined the role of IPL in primary dermatologic diseases. They gave a moderate recommendation for IPL in the treatment of erythematotelangiectatic rosacea, noting that its efficacy is comparable to the use of the pulsed dye laser.
Photo copyright Getty Images.
[pagebreak]
Dr. Lupo uses IPL for diffuse redness, but turns to her Cutera Excel V 532nm/1064nm vascular laser for discrete telangiectasia. “If they are visibly discrete, well defined and if they are at all within the purple range, you’ll need the 1064nm laser,” she says. “For the most minimal telangiectasia, you may get some improvement with IPL, but it’s not optimal. This is partly due to the spot size and the way the handpiece is designed.”
The large, stamp handpieces of IPL devices do limit their utility in treating visible vessels on the face. “Most of them have very large spot sizes, so it’s a little bit difficult to treat in small areas like the nose, the lips and around the eyes with the handpieces we have right now,” says Jason Emer, MD, a dermatologic surgeon with the Roxbury Institute in Beverly Hills, California, who uses IPL as a preventive, maintenance treatment for fair-skinned patients in his practice. “That’s certainly one shortcoming of these devices.”
Melasma. IPL has become the first line of treatment for both pigmentation and melasma in Asia and is widely used for these indications in the U.S. as well, according to Dr. Gold. “There is no cure for melasma, but with the right settings and the right filters, you can successfully treat it in many cases,” he says.
The literature review by Dr. Goldman and colleagues suggested a strong recommendation for the use of IPL in combination with topicals for the treatment of melasma in skin types I-III. They note that it may be preferable to the Q-switched alexandrite laser when treating Asian patients for pigment concerns due to a lower risk of post-inflammatory hyperpigmentation (PIH).
Despite its relative safety, Dr. Emer cautions that IPL does pose a risk of PIH in both olive and darker-skin toned patients. To reduce the risk, he often combines low-energy IPL with low-density resurfacing lasers or fractional radiofrequency (RF) to treat melasma. “You can do a very light IPL on the pigmented areas and then do a light, low-energy, low-density treatment with the Clear + Brilliant laser, or the Venus Viva or Skinfiniti RF devices. The RF technologies are better for sensitive skin types III-V because they don’t increase the risk of hyperpigmentation.”
Acne. IPL can be used both alone or as a light source for photodynamic therapy (PDT) in the treatment of acne. Dr. Goldman and colleagues made a moderate recommendation for the use of IPL alone to treat acne and a strong recommendation for its use in PDT where it showed an efficacy rate of 60% to 80% improvement compared to 40% to 60% improvement when IPL was used alone.
“All of the IPL companies are getting into the acne treatment market now with new treatment protocols and cut off filters,” says Dr. Gold.
Off-the-face skin rejuvenation. “One of the biggest advantages of IPL is that it can be used all over the body,” says Dr. Emer. “Lasers have the potential to cause burns and scars, and although IPL can cause blistering, the risk is lower and you can get really good results with pigmentation on the chest, arms, back and shoulders.”
In the U.S., it has become a popular treatment for Poikiloderma of Civatte. “This is actually dilated vessels in the dermis and pigment deposition into the dermis, and IPL lets you address both of these things with one handpiece, so it has become a huge indication for IPL,” says Dr. Gold.
Dr. Lupo does urge caution when working off the face. “Delayed healing is more likely because of the lack of sebaceous glands,” she says. “I’ve seen bad complications, particularly on the legs when it was used for hair removal on a darker skin type—III or higher—because the provider didn’t use a high enough cut off filter or opt for the 1064nm laser.”
Photo copyright Getty Images.
[pagebreak]
Today’s IPL devices offer several advances over those of yesteryear, most of which are geared toward to reducing adverse events and improving efficacy. “The biggest advance in IPL technologies today is what we call ‘squaring of the pulse,’” says Dr. Gold. “In the early days, in order to get the energy to deliver across the pulse length, you needed a big burst of energy to start—about 30J/c2 to 40J/c2—and that dissipated rather quickly. That’s where we got a lot of burning, especially when combined with less sophisticated cooling.”
Lumenis developed Optimal Pulse Technology (OPT), which squares the pulse so you get the same amount of energy throughout the entire pulse—this technology has since been adopted by most large IPL and laser companies.
“Instead of using 30J/c2 to 40J/c2 of energy, we’re now using 12J/c2 to 14J/c2 and getting the same, if not better, results because the energy is going the entire length of the pulse,” says Dr. Gold.
When IPLs first came to the market, there was no built-in cooling; instead practitioners applied cold gel, which acted as both a cooling agent and a conductor of energy. “We still use gel to help get the energy through to the skin, but most devices now have some kind of sapphire-guided cooling mechanism to protect the skin,” says Dr. Gold.
Additional safety improvements include temperature and impedance monitoring. “In the past, you had quick bursts of energy and if your handpiece wasn’t perfectly on the skin or you didn’t have enough gel, you could get blistering,” says Dr. Emer. “Now some of the technologies measure the temperature, so that if the handpiece is not perfectly on the skin when it fires, it won’t fully fire the energy.”
Companies are also adding cut off filters to target specific concerns, such as acne (400nm range) and vascularity (500nm to 600nm). “The devices are getting much more sophisticated in how they deliver the energy and in making the filters more precise. Sciton was the first company to create an acne filter, and now this is happening across the board,” says Dr. Gold.
The cut off filters also improve safety by allowing providers to vary wavelengths based on skin type. “If I have a patient who is a lighter skin type III, and I do think IPL would benefit them, I would use the 590nm or 615nm cut off filter, and that increases the safety greatly,” says Dr. Lupo. “As a rule, the fairer the patient the lower the number you can use.”
Despite new safety features, complications do occur with IPL. The most common adverse events are skin burning and blistering. “You have to understand skin healing,” says Dr. Lupo. “Anyone who uses these devices can have complications; the key is understanding how to manage a complication, which means understanding the physiology of the skin and the basics of wound healing. If the patient is in pain, the energy is too high. Anytime you see graying or whitening of tissue, that’s a very bad sign, and if you see the skin lift or extreme redness—like when you touch your arm with a curling iron—that is a burn. The skin will blister over the next few hours, so know your clinical endpoints and what you are observing.”
Photo copyright Getty Images.
[pagebreak]
Proper stamping technique will also help prevent poor outcomes. “Make sure the tip is not directly on bare skin. You want it to somewhat float over the layer of gel, so that the gel cushions it and prevents it from leaving stamp marks,” says Dr. Lupo. “When you have a stamp device that you’re lifting and repositioning, it’s very important that you have a methodology of overlap—about 10%—and continuity of care so that you don’t end up with a lot of streaking or gaps in the treatment area. Streaking is temporary, and you can get it on the next treatment, but it shows a lack of precision and care.”
In many practices and medspas, IPL treatments are delegated to NPs, PAs, RNs or even estheticians. In addition to providing proper training, the supervising physicians should also be familiar with the device and proper usage. “Too often I see a practice buy a device and then hand it off to an employee, and then those patients end up scarred in my office. That can happen with any device, but we know it happens in the IPL world,” says Dr. Gold. “When you turn on an IPL, there are so many options—from pulse widths to cut off filters—and so many variables. It really is the thinking person’s device compared to certain lasers, so you must have training and continuing education for the staff and the supervising physician.”
Is IPL for You?
With so many light- and energy-based devices on the market, practices must determine which technologies will get the most use and provide the best benefits to patients. The versatility of IPL makes it a good choice for facilities that don’t already have a wide range of lasers. “If your skin type population is mostly Caucasian, an IPL is an excellent first device for a new practice because it’s a very good, very versatile device and usually on the less expensive end of the range,” says Dr. Lupo. “My major caution is, just because you have an expensive hammer, not every concern is a nail. Each device has a niche; each has strengths and weaknesses. If you don’t have the optimal device for a patient’s concerns, you should refer them to someone else. As your revenue grows with the IPL, then you can invest in additional lasers or skin tightening devices.”
IPLs are available at a wide range of price points. If you are investigating devices, do ask about safety features and versatility. “Cheap IPLs are cheap—I can buy an IPL for $5,000 or I can buy an IPL for $100,000,” says Dr. Gold. “The question is, what are you getting for the $5,000; and the answer is a light. At the higher ends, you’re getting more safety features and years of experience behind the technology. If you find the right device, get training and then follow the guidelines, these are the easiest, most versatile devices to use.”
Inga Hansen is the executive editor of MedEsthetics.
Photo copyright Getty Images.