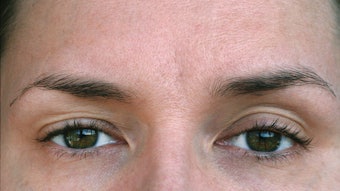
Patients who suffer from rosacea may exhibit any number of uncomfortable symptoms, from flushing and dilated capillaries to papules, pustules and ocular irritation. Treatment options similarly vary, as do theories as to what the underlying causes of rosacea may be. While recent research highlights cardiovascular links and explores the potential role of facial microorganisms, experts agree that the best treatments for rosacea target the chronic inflammation of the skin and body, and require a holistic approach to patient care. Patients most commonly present with erythematotelangiectatic rosacea—flushing, redness and dilated capillaries—and some develop papules and pustules as well. “It’s the redness and visible vessels that have traditionally been the more difficult aspect to treat,” says New York City-based dermatologist Diane S. Berson, MD. “Patients with rosacea tend to have skin that’s very sensitive and very easily inflamed.”
Causes and Triggers
While physicians and researchers now have a more thorough understanding of how certain triggers cause flare-ups in patients with rosacea, the specific cause of the disease has not been identified.
“There are many different inflammatory mediators involved with the pathogenesis of rosacea, and every day we’re learning more,” Dr. Berson says. “Triggers may stimulate increased innate immunity, inflammation and vascular hyperactivity.”
“Over the past several years, we have learned a lot about how and what the trigger factors of rosacea are causing,” says Julie C. Harper, MD, president-elect of the American Acne and Rosacea Society and private practice physician at the Dermatology and Skin Care Center of Birmingham in Birmingham, Alabama. “An up-regulation of the innate immune response has garnered the most attention, with an increase in toll-like receptor 2 (TLR2) and cathelicidin activity in rosacea-prone skin ‘turning on’ inflammation. A trigger—such as Demodex mites or the bacteria in Demodex—activates TLR2, which in turn triggers cathelicidin. And cathelicidins, such as LL-37, promote inflammation in the skin.”
Dr. Harper notes that some transient receptor potential channels (TRPs) also may play a role in the development of rosacea. “Certain TRPs mediate a response to spicy or hot sensations in the skin, leading to a neurogenic vasodilation,” she says.
The theory that Demodex mites trigger inflammation is a popular one, though how or why they may affect rosacea is unclear. “I think that people who believe rosacea is caused by Demodex mites are a little mono-focused,” says Mary Lupo, MD, founder of the Lupo Center for Aesthetic & General Dermatology in New Orleans. “We all have Demodex mites—but there’s a subset of people that mounts a more robust inflammatory response to them.”
Cleveland-based scientist and dermatologist Daniel Popkin, MD, PhD, is similarly skeptical of the research— though antimicrobial/antiparasitic topicals such as ivermectin kill the mites and appear to work, a crucial step was skipped. “There are associations with this mite and rosacea, and indeed the ivermectin cream works, but the researchers never actually looked at mite counts. It would have been a good opportunity to address the relationship between mites and rosacea,” he says.
Photo copyright Getty Images.
[pagebreak]
Rosacea typically affects patients with lighter skin types, particularly skin types I and II (though it does occasionally affect darker-skinned patients too). It’s no surprise then that in his research on genetic and environmental contributions to rosacea, Dr. Popkin found that the main risk factor was sun exposure, followed by the patient’s age. “The biggest driver by far was sun exposure, and then age was also an independent predictor. They are obviously co-linear in the sense that as you get older you have more cumulative sun exposure, but even independent of each other there was a signal there,” he says.
It’s not uncommon for rosacea triggered by sun exposure to also result in photo damage—increases in inflammatory mediators lead to increases in free radical production. “Patients with rosacea tend to have concomitant photo damage; erythema develops as a result of free radical production, subsequent inflammation and chronic sun exposure, which leads to collagen degradation,” says Dr. Berson. “These patients with sensitive skin have compromised barrier function, chronic oxidative damage and increased blood flow to the skin.”
Sun exposure is also one of the most common triggers for rosacea flare-ups. Other triggers include extreme temperatures, alcohol, spicy foods and exercise. “It’s unfortunate because exercise, otherwise beneficial, can exacerbate redness, flushing and discomfort,” says Dr. Berson.
Healing the Skin Barrier
Calming rosacea typically requires a combination approach, including topical and oral prescriptions, adjunctive aesthetic procedures and dietary changes. But providers must first address the patient’s compromised skin barrier.
“You need to discuss the cosmeceutical protocols that a patient is on, because one of the main things that further inflames a sensitive lipid barrier is the barrier disruption that occurs in rosacea as a result of the inflammation. It’s a ‘chicken and the egg’ situation—the disrupted barrier further exacerbates the rosacea, and so forth,” says Dr. Lupo. “The single most important thing (non-prescription wise) is to make sure you repair the patient’s barrier—make sure they are using anti-inflammatory products that decrease transepidermal water loss (TEWL).”
Because these patients have lost barrier function, providers should look for gentle cleansers and emollient moisturizers with hydrating or humectant ingredients— such as lipids, ceramides, heparan sulfate, glycerin and hyaluronic acid—to help restore it. Dr. Berson adds that anti-inflammatory and antioxidant ingredients such as niacinamide (vitamin B), resveratrol, and vitamins C and E are beneficial for compromised skin as well.
“Simply restoring the barrier may help decrease flares as the patients are less sensitive to potential irritants,” says Dr. Berson. “Recommending the appropriate skin care will make them not only respond better to their treatment but will also help maintain clear skin.”
Additionally, sun protection is mandatory for rosacea patients. “I like the physical sun blocking agents with inorganic ingredients such as zinc and titanium,” says Dr. Berson. “We combine sun block agents with antioxidants in the morning, further protecting the skin by decreasing oxidative damage and free radical production. This can also help protect the skin from the effects of heat and infrared light, which contribute to inflammation and photo damage.”
Photo copyright Getty Images.
[pagebreak]
Prescriptive Care
Popular prescription topical treatments for rosacea patients include Finacea Foam (azelaic acid, Bayer) and metronidazole for papules and pustules, Mirvaso (brimonidine, Galderma) for redness and Soolantra (ivermectin, Galderma), which targets Demodex mites. Papulopustular inflammation may also be managed with some of the same treatments for acne, such as topical antimicrobials or antibiotics.
“My No. 1 prescription topical is Finacea Foam,” says Dr. Lupo. “I participated in the clinical trials, so I saw firsthand very early on how beneficial and well tolerated it was.”
“Azelaic acid may have some anti-inflammatory and antimicrobial properties, and it might also decrease some of the inflammatory mediators,” says Dr. Berson. “Topical ivermectin has a dual mechanism of action—targeting Demodex mites and also having anti-inflammatory properties.”
Mirvaso, on the other hand, is a vasoconstrictor that works on blood vessels that have muscular lining. Dr. Berson finds that effects can be seen half an hour after application, and though they last for about a day, the effects peak at around six hours. “It won’t work on the superficial telangiectasia and capillaries, because they don’t have a muscle lining,” she says. “So those little vessels will still be there, but constricting the muscle lining of some of the bigger vessels will decrease redness by decreasing the blood flow.”
She also points out that Mirvaso is a cosmetic therapy. “It’s for patients who want to look less red—it does not treat the underlying problem, and at the end of the day patients go back to their baseline redness,” she says.
In addition to topical treatment, low-dose doxycycline (Oracea, Galderma) is an effective oral medication that is antimicrobial and anti-inflammatory. “Oracea is the optimal medicine orally, because it has a sub-antimicrobial dosage, which means it’s purely anti-inflammatory,” says Dr. Lupo. Patients don’t have to worry about developing a resistance, which makes it ideal for more severe cases where they need long-term oral medication.
“Although it’s approved for the papules and pustules of rosacea, anecdotally we do see some improvement in the redness of rosacea with Oracea,” adds Dr. Berson.
Oral antibiotics as well as topical cyclosporine emulsion may also be used in the case of ocular symptoms, says Dr. Harper.
In-Office Support
As part of her holistic approach to treating rosacea, Dr. Lupo actively discusses diet with her patients. Her anti-inflammatory regimen includes omega 3 supplementation and a diet low in alcohol, carbohydrates and sugar. “More than any other condition, I see improvement in rosacea when patients improve their diets,” says Dr. Lupo.
Adjunctive in-office treatments, such as salicylic acid peels, intense pulsed light (IPL) and laser procedures, may provide faster relief for rosacea patients as well.
Photo copyright Getty Images.
[pagebreak]
Salicylic acid, which is related to aspirin and therefore anti-inflammatory, will certainly calm the papulopustular component and may also soothe redness. “I perform salicylic acid peels on rosacea patients who are red, ruddy or inflamed and maybe have some papules,” says Dr. Berson. “It helps calm the skin, gives patients a ‘glow’ and may improve the appearance of their pores, while subtly improving tone and texture.”
For erythema and telangiectasia, Dr. Lupo will use IPL or the excel V (Cutera) 532nm laser, and Dr. Berson similarly offers VBeam Perfecta (Syneron Candela) treatments. “These lasers can target both the vessels and the redness. I typically use a 10mm spot size, from 7J to 7.5J and 10ms pulse width,” says Dr. Berson.
IPL and vascular lasers will offer quick relief, though it is temporary, notes Dr. Harper. She counsels her patients that they can conceal erythema and papules with makeup as well.
Of note, dermatologists have been anecdotally noticing improvements in flushing when they inject neurotoxin into these patients. “There are increased neurotransmitters in patients with rosacea, therefore flushing may be another potential target for neuromodulators,” says Dr. Berson. “Patients notice an improvement of their flushing and oiliness in areas injected. I wouldn’t call it a treatment at this point—just an observation when we’re injecting rosacea patients with neurotoxin.”
Ongoing Research
Though there are a number of ways to calm and treat the symptoms of rosacea, the underlying cause is still unclear beyond the fact that it’s an issue of chronic inflammation. “It’s a growing field in terms of understanding what rosacea is and the best way to treat it,” says Dr. Popkin. “So in some ways what we have in our tool box is relatively primitive, and it reflects the absence of our knowledge. Even with a common topical like metronidazole—it’s an antibiotic, but we don’t really know how or why it’s working.”
Dr. Popkin and his colleagues are currently studying the facial microbiomes of twins in which only one of them has rosacea. “We did swabs on the left and right cheeks of different twin pairs, and we then sequenced their microbiomes,” he says. “Essentially we’re trying to look for any type of correlation between the bacteria on their skin and the severity or absence of their rosacea.” Their data is still being analyzed and this particular study has not yet been published
In August 2015, the Journal of the American Academy of Dermatology (JAAD) published a study from Taiwan in which researchers found that dyslipidemia, coronary artery disease and hypertension were significantly associated with rosacea. Coronary artery disease remained independently associated with rosacea after adjustment for hypertension, diabetes mellitus and dyslipidemia.
Dr. Lupo has seen the link between cardiovascular disease and patients with rosacea and psoriasis for many years in her practice. She attributes it to inflammation and it’s why dietary supplements, particularly omega 3s are standard protocol for her rosacea patients. “Omega 3s are very important for preventing cardiovascular disease and I do see a link to cardiovascular disease in both rosacea and psoriasis,” she says. “I think it’s that pro-inflammatory environment of the patient.”
Dr. Harper also points out that tetracycline antibiotics such as Oracea, may help reduce cardiovascular risk in addition to easing rosacea symptoms.
“Cardiovascular comorbidities are being reported in association with dermatologic conditions whose root cause involves inflammation, including rosacea psoriasis and possibly eczema,” says Dr. Berson. “It will be interesting to see what we as dermatologists can do for our patients to improve their inflammatory skin conditions and how this might have a potential positive impact on an underlying cardiac risk they might have had. I don’t know that we know the answer yet, but it’s certainly food for thought.”
Laura Beliz is the associate editor of MedEsthetics.
Photo copyright Getty Images.