Much has been written about how to attract prospective patients to one’s aesthetic practice, but bringing consumers in the door is only the beginning. Once a consultation has been booked, medspas and cosmetic practices must be able to identify a prospective patient’s specific concerns and aesthetic goals, and be prepared to effectively communicate both recommended treatment options and why their team is qualified to help the patient achieve these goals.
Here, physicians and aesthetic business consultants share their top consultation strategies and advice to help practices improve their patient conversion rates.
Identifying Concerns
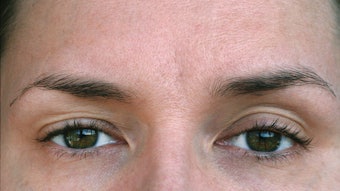
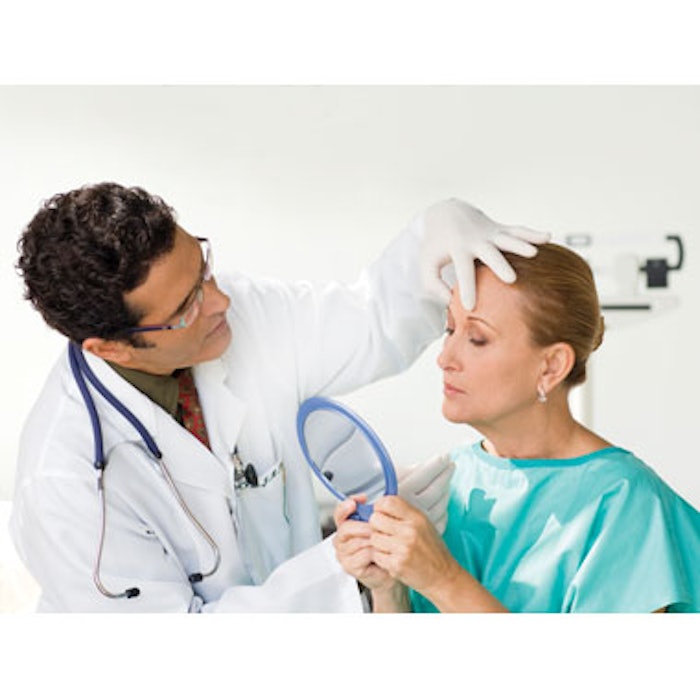
The first step in a successful consultation is properly identifying the prospective patient’s aesthetic concerns and goals. In addition to cultivating good listening skills, providers often incorporate tools, such as mirrors, questionnaires and imaging technologies to help facilitate communication.
Ruth Tedaldi, MD, founder of Dermatology Partners in Wellesley, Massachusetts, hands every patient a mirror at the beginning of the consultation and asks them to point out their concerns. “I use the mirror to establish what is objective and what is subjective,” she says. “Every patient has a concept of what they don’t like, but they may not know how to correct the defects. By showing them that the area or feature they’re unhappy with is actually affected by a relationship to another feature, you can educate the patient and instill confidence in your ability to fix the problem.”
H.L. Greenberg, MD, founder of Las Vegas Dermatology in Las Vegas, finds that handing patients a mirror and asking them to explain their problem areas will often lead them to share concerns beyond the one for which they originally booked the consult. This allows you to prescribe the most effective treatments for their overall goals. “Brutal honesty is important during the evaluation,” he says. “By using the mirror, we can identify every flaw or concern in the potential treatment area before making recommendations.”
“Mirrors are the greatest silent selling tool,” says Catherine Maley, MBA, president of Cosmetic Image Marketing in Sausalito, California, and author of Your Aesthetic Practice: What Your Patients Are Saying. “Give every patient a hand mirror that they can control and have wall mirrors throughout the office. This helps prospective patients zero in on why they are here at your practice.”
Kimberly Bertrang, LPN, owner of Allure Skin Health in Sun Prairie, Wisconsin, asks new clients to complete a questionnaire prior to the consultation. Among the most important questions are “What is your concern?” and “Who referred you?” “Knowing who referred the client is helpful, as people often are compelled to come in because they have the same concerns and expectations as the person who referred them,” she says.
In contrast, Dr. Tedaldi has chosen not to use questionnaires. “I don’t want to read what the patient filled out on a piece of paper,” she says. “It is my job as a physician to assess the patient, make treatment recommendations and help them choose the best procedure—even if it’s not what they were thinking about—based on their budget, health and other factors.”
Image: Getty Images.
[pagebreak]
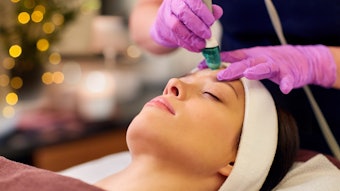
Prescribing Treatment
Once you are clear on the patient’s primary goals, the next step is to make your treatment recommendations. Offering patients multiple options, typically at a variety of price points with differing downtime requirements “helps them to make their own decisions,” says Bertrang. “Furthermore, I don’t point out defects as I look at their skin. Rather, I talk about how the procedures will benefit their skin, and help to prevent and correct their concerns.”
When reviewing treatment recommendations, Dr. Greenberg encourages physicians to be honest and upfront about costs, number of sessions required and potential outcomes and complications. “As cliché as it sounds, under-promising and over-delivering is a great way to set realistic patient expectations and to prevent patients from being upset,” he says.
Dr. Greenberg regularly employs his Visia Complexion Analysis system (Canfield Scientific) to identify skin concerns and direct product recommendations. “Having a great
picture of the patient’s own skin will enhance sales opportunities,” he says.
Systems that include treatment simulations of surgeries and filler treatments, such as the Vectra 3D imaging system (Canfield Scientific), can also help improve conversion rates and patient satisfaction. “Simulations are good for breast augmentation, facial implants or rhinoplasty—any procedure that changes physical structure,” says Stanley G. Poulos, MD, of Plastic Surgery Specialists in Marin County, California. “It allows for a clearer conversation between the surgeon and patient. I can show the patient preoperatively what the surgical result will look like on her body.”
“There is nothing better than imaging systems to tell the story of what outcomes you can achieve,” agrees Cheryl Whitman, author of Beautifully Profitable/Forever Profitable and CEO of national aesthetic business consulting firm Beautiful Forever. “Today’s aesthetic patients want to know what the end result will look like, and it helps to manage their expectations.”
More than 90% of the cosmetic patients that Maley has interviewed say they want to see computer simulations during their consultations. “It’s far more compelling when a patient sees a potential outcome of her own rather than someone else’s photos,” she says.
But use caution, Dr. Tedaldi advises. “Be wary because simulations are not always 100% accurate—especially those that show a patient what a little extra volume or contour change would look like,” she says.
Practices that do not currently have imaging systems can still help patients see potential outcomes of treatment by manipulating the patient’s own features in a mirror, and by sharing before and after images of previous patients. “Show the patient what she can achieve by manipulating her face in the mirror to show results,” says Whitman. “Using the mirror, explain what is causing the issue and how you can correct it.”
Although you can’t accurately simulate what a procedure will feel like, you can share other patient’s descriptions as well as procedure animations to help prospective patients understand the process. Dr. Poulos’ practice website contains 3D animations of common aesthetic surgeries for patients to view. He discourages posting actual surgical videos, as they are too graphic for most patients.
Image: Getty Images.
[pagebreak]
To help patients understand the pain level as well as the outcomes that can be achieved with a recommended treatment, Dr. Greenberg will treat a single skin tag, sebaceous hyperplasia or lentigo with the chosen device, or inject the nasolabial folds with saline to demonstrate the action and outcomes of dermal fillers.
In order to establish credibility with prospective patients, plastic surgeon Joseph O’Connell, MD, principal and founder of The Aesthetic Center in Westport, Connecticut, gives prospective patients copies of scientific articles he has written on the procedures they are seeking.
Key to establishing trust is making sure that the prospective patient feels you understand her unique concerns in terms of desired outcome, budget, pain and downtime. “You have to sense a patient’s needs so you can be a better physician in each situation—it’s a dance,” says Dr. Tedaldi. “The physician who treats every case with the same format won’t be as successful as those who craft individual, unique treatment plans for each patient.”
Booking the Procedure
Once the consultation has ended, it is time to ask the patient if they would like to book treatment. This can be the most uncomfortable portion of the consult for many providers, which is why Whitman recommends enlisting the help of a staff member, typically the patient coordinator. “This person acts as the ‘closer.’ He or she discusses the price of the agreed-upon procedure and sets up the appointment,” she says.
At Dr. Poulos’ practice, a patient care coordinator meets the patient first (prior to the consult) and credentials the practice by providing details about the provider’s training and experience. After the consultation, the coordinator discusses the treatment recommendations with the surgeon, then meets with the patient to review costs, financing options, scheduling and recovery.
Dr. O’Connell and Dr. Tedaldi also defer discussion of costs and financing to a patient coordinator. “It isn’t my job to determine what someone can or cannot afford or how to pay for it,” says Dr. Tedaldi. “I present all the treatment possibilities and explain expected and unexpected side effects. However, it’s also important for the patient to have an idea of a treatment’s cost and the potential need for further treatments. My cosmetic director explains the concept of full correction and the costs associated with it.”
Having a patient coordinator or cosmetic director on staff is also helpful because the practitioner isn’t always available, says Dr. Tedaldi. “Questions may arise after the consult when the physician is already seeing the next patient, so it’s an extension of your abilities to have someone else available and able to answer follow-up questions,” she says.
When it’s time to discuss costs and payment options, Whitman recommends offering a small discount for paying cash and working with a financing company for patients who want to break up their payments over time. “Use the marketing materials provided by companies, such as Care- Credit or LendingUSA,” she says. “When looking at the rates and repayment schedule, break down a daily payment schedule for the patient to show how little the actual cost will impact her.”
Zero interest financing options have increased conversion rates in Dr. Poulos’ practice because they allow patients to budget the costs of high-priced procedures that might otherwise be unaffordable.
At Allure Skin Health, patient financing has caused some conflicts, says Bertrang. Complaints typically relate to higher-than-expected interest rates. So do investigate financing companies carefully and make sure patients understand the terms of the agreement.
Image: Getty Images.
[pagebreak]
Following Up
If a prospective patient chooses not to book a procedure after her consultation, practitioners must decide what type of follow-up is appropriate. “If a patient is about to leave without booking an appointment, I would establish a day to follow up with them before they go,” says Whitman.
The providers we spoke with are split on whether follow-up phone calls or emails are appropriate. Dr. Tedaldi does not want to pressure patients into having procedures. “Our job is to educate, not to try and woo them into doing something,” she says.
Dr. O’Connell doesn’t think follow-up communication is useful and views it as a potential violation of their privacy. “Sometimes the person’s spouse may not even know they came in,” he says.
Conversely, Bertrang sends a handwritten thank you note about 10 days after the consultation that includes something specific that was discussed. “I don’t point out their concerns, but rather discuss preventative care and benefits,” she says. “I ask them to call if they think of more questions.”
Dr. Poulos has found that prospective patients often appreciate follow-up calls or emails from the practice’s patient coordinator, and some credit the additional follow-up as the reason they finalized their decision to proceed. “Our coordinators maintain contact with potential patients until they tell us not to,” he says. “Our practice management software provides tracking ladders that allow our coordinators to do this efficiently.”
Maley applauds this strategy. “You must follow up because there’s a chance the patient is ready to move forward, especially with a little nudge from you,” she says.
Karen Appold is a medical writer based in Pennsylvania.
Image: Getty Images.