When we talk about deep chemical peeling, the first names that come to mind are Baker-Gordon. Although dermatologists and plastic surgeons have been using ingredients, such as phenol and croton oil to reduce scars and rejuvenate aging skin as far back as the mid-1800s and early 1900s, it was the work of Thomas Baker and Howard Gordon in the 1960s that brought phenol-croton oil peels mainstream. But just 30 years later, deep chemical peeling waned in popularity due to the potential for cardiac complications and the introduction of new laser skin-resurfacing technologies.
Today, there is renewed interest in deep chemical peels thanks to another pioneer, plastic surgeon Gregory Hetter, MD, and a new generation of dermatologists and plastic surgeons who are spearheading safer, segmental approaches that combine deep and medium-depth medical peels.
“New developments in chemical peeling, especially in the past five years, have radically changed the way doctors perform deep peels,” says Hal Brody, MD, of Atlanta Dermatology and clinical professor of dermatology at Emory University School of Medicine.
Safer Formulation
Believing there was a better, safer way to perform medical peels, Dr. Hetter began studying phenol and croton oil deep peels in the 1980s and published several papers in 2000 outlining his discoveries. He found that the croton oil, not the phenol, is the active ingredient that rejuvenates skin. He also concluded that the concentrations of both phenol and croton oil used by Baker and Gordon were significantly higher than needed for efficacy, leading to unnecessary risks to the patient.
“The old formulas used by Baker and Gordon, which were the classic formulas for deep peels, had a 55 percent phenol and 2.1 percent croton oil concentration, which is very, very strong,” says Carlos Wambier, MD, a private practice physician from Brazil and post-doctoral associate at Yale University. “You do not need that much of either ingredient to achieve rejuvenation.”
In what is now called the Hetter formulation, the concentration of phenol is 35 percent and the concentration of croton oil varies from 0.1 percent to 1.6 percent based on the concern you are treating. “If I am treating deep wrinkles, I go to 1.6 percent; if the skin has few wrinkles and we just want a tightening effect, we use 0.1 percent,” says Dr. Wambier.
Croton oil, derived from the Croton tiglium seed, has a long history in Indian medicine. “It has been used for hundreds of years, and when croton oil is dissolved in phenol and this is, in turn, emulsified into water, it creates a special kind of delivery system,” says John Kulesza, founder and chemist, Young Pharmaceuticals.
Croton oil alone cannot penetrate the superficial layers of the skin, but the small phenol molecule can reach the deep layers of the dermis and enter the bloodstream. When the two are mixed, the phenol delivers the oil to the deep layers of the skin where it exerts a strong inflammatory and rejuvenating effect.
“The croton oil makes this magic that we’re still trying to understand,” says Dr. Wambier. “It causes intense inflammation and acts as a fertilizer for skin regeneration. Inflammatory cells flood the whole dermis, and they hunt for anything, including any cancers. They sweep the existing skin and then new skin forms—but it’s younger skin with more elastin fibers and more collagen. That is the action of croton oil. It’s not a burn.”
The lower concentration of phenol in the Hetter formulation reduces the risk of toxicity and scarring. “Now we can give patients more safety in regards to risk of scarring, particularly in the neck and eyelids where the skin is very thin. In the past, we would never do a deep peel in those areas,” says Dr. Wambier.
“By decreasing the percentages of both phenol and croton oil, these peels are safer,” says Dr. Brody. “A full-face peel still requires cardiac monitoring, but what we have learned is that we can do segmental peels, where we peel one area at one depth and another area at another depth.”
Segmental Peels
Segmental peels typically combine deep peeling in small areas of severe wrinkling with a medium-depth peel on the rest of the face to address moderate damage and prevent lines of demarcation.
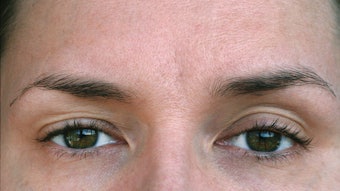
“People today smoke less and expose themselves to the sun less than they did 30 years ago, so we don’t see these severely photodamaged, very wrinkled faces that we used to,” says Dr. Brody. “But around the mouth and eyes, especially, we still see areas that need to be deeply peeled, and these peels are successful in removing all the lines around the mouth, which is something fractional lasers are not capable of doing.”
Because the phenol-croton oil peel is used in such a small area, patients typically do not require cardiac monitoring or IV hydration when undergoing segmental peels. “We can do the hydration orally and we can do the sedation orally, so it is much safer,” says Dr. Brody.
Kachiu Lee, MD, director of the Brown Dermatology Laser and Cosmetic Center in Rhode Island and assistant professor of dermatology at Brown University, frequently combines deep peeling with medium-depth peels. “Especially for women, their lines may be much deeper around the mouth or around the eyes, so I might do a deep chemical peel for the mouth or eyes and then a medium-depth peel for the rest of the face to make sure the color is even,” she says.
The two most commonly used medium peel formulations are dry ice followed by trichloroacetic acid (TCA) or Jessner’s solution followed by TCA. “These are tried-and-true medium peels that are excellent at blending other areas,” says Dr. Brody.
“The point of that first step—whether with Jessner’s or dry ice—is that it causes epidermal sloughing, and that allows the TCA to penetrate deeper,” explains Dr. Lee. “It’s very safe. You don’t need any monitoring.”
The Lip Peel
Dr. Wambier introduced the deep lip peel, a noninjectable lip augmentation procedure, at the International Peeling Society meeting held in Washington, DC, on February 28. “The most interesting thing about the lip peel is that it not only gives volume and eversion, things we always try to get with fillers, but it treats the skin of the lips as well,” he says.
The entire procedure takes about four minutes and does not require anesthetic. “There is an initial sensation like pepper on the lips and then, after three seconds, the lips are numb because phenol is a numbing agent,” says Dr. Wambier.
Patients use Vaseline on the lips for the first 10 days but can eat and drink within an hour of the peel. “About 12 hours after the peel, the lips become very swollen. The swelling fades in one to two days. Sometimes there are some blisters and some oozing, but that only lasts the first two to three days,” says Dr. Wambier. “Because the lips heal so fast, by the fourth or fifth day, the patient is well and can do whatever they want.”
He has been performing this procedure for eight years and notes that his patients still retain volume and eversion.
“For younger patients who are healthy and not on medication, it is completely safe to do this procedure without monitoring and without IV, because the lips are so small,” he says.
Cardiac Cautions
The size of the area treated is the primary factor in determining whether a patent needs cardiac monitoring: It must be less than 1 percent of body surface area. “Below 1 percent and particularly below 0.5 percent body surface area—the palm of the hand without the fingers is 0.5 percent body surface area—it is safe, depending on the patient, of course, to do a peel without cardiac monitoring because there is minimal exposure to the chemicals,” says Dr. Wambier. “Once you get over 1 percent body surface area, the risks start to increase.”
Patient medical history is the second factor to consider. For patients who have a history of cardiac events, Dr. Wambier uses monitoring regardless of the area treated.
“If someone has a cardiac arrhythmia or they are very elderly or taking medications that can cause arrhythmia, I would monitor even for very small areas,” he says.
If you are deep peeling multiple areas—the perioral, periorbital and between the eyes, for instance—or performing a full-face deep peel, patients do need cardiac monitoring and IV hydration. Patients who have a history of arrhythmia as well as those who are taking certain medications may be poor candidates for the procedure.
Prior to a full-face deep peel, Dr. Lee has the patient undergo an EKG and get clearance from their primary physician. “We also review their medications to make sure they are not on any medications that can prolong the QT interval,” she says. “Some of the psychiatric medications can prolong the QT interval, also some of the anti-arrhythmia medications, such as amiodarone, and some antibiotics and antifungals.”
If the patient’s medical conditions are well-managed and the EKG is normal, “I am comfortable peeling them,” says Dr. Lee.
To reduce the risk of cardiac events, the peel is performed slowly. “We use pauses,” says Dr. Wambier. “We peel the forehead, take a 10-minute pause, move on to the next area and then we take another pause. This gives time for the systemic absorption of phenol and croton oil to be eliminated in the urine. We take over one hour to peel the whole face even though we could do it in five minutes. This allows us to monitor what is happening and if we see something changing on the cardiac monitor, we can stop the peel or provide medication.”
Pre- and Post-Care
Whether the patient is undergoing a full-face deep peel, lip peel or segmental peel, “herpes is the main complication we are concerned with,” says Dr. Wambier. “People can be infected with HSV for years and never have an outbreak, but when we do the peel, it activates the nerves and can cause an outbreak. So we use prophylactic antivirals for all patients.”
“Pre- and post-op, it’s very similar to a laser procedure,” says Dr. Lee. “We put them on antiviral medications to prevent cold sores, prescribe antibiotics as needed, and follow up regularly to make sure they are healing properly. I have them do vinegar soaks, because it’s a natural way to prevent bacterial infection.”
Dr. Wambier applies Vaseline after the procedure and counsels patients to keep using it for 10 days. “After that, they usually can go back to their normal daily moisturizer and sunscreen,” he says.
For a week following the procedure, he has them come in every day to monitor healing. “If there is oozing in one area, foul smell or pain—or if one area of the face just feels different—this could be an infection, and you want to catch this right away,” says Dr. Wambier. “If there is infection, we prescribe oral antibiotics but we do not use prophylactic antibiotics.”
Patients can expect some oozing for the first day and pain in the first hours following the peel. “Because the phenol is an anesthetic, the patient has pain about 30 minutes after the procedure that lasts for about six to eight hours,” says Dr. Brody. “We do all these procedures in the morning so that by suppertime and bedtime, they have no discomfort.”
Patients will experience redness and post-inflammatory hyperpigmentation (PIH) in the weeks and months following a deep peel. “PIH and erythema are part of the treatment. Every patient has it, so these are to be expected,” says Dr. Wambier. “The patient will be red for a month. As soon as the redness starts to fade, we will see more pigment. But around six months after the peel, that hyperpigmentation is gone and the skin is fully recovered.”
Skin Type Considerations
The risk of long-term PIH is significantly higher for patients with darker skin and those of specific ethnic backgrounds. “But most people with darker skin tones don’t have this degree of wrinkling,” says Dr. Brody. “We don’t see deep wrinkling in patients who are African-American or Endo-Pakistani, for example, so you would use the lower strength of the phenol-croton oil solutions. Medium depth peels are generally only done in light to medium-dark skin types.”
Due to the risk of PIH, Dr. Lee recommends that only doctors with many years of experience perform deep peels on skin types III and IV. “Some very experienced doctors deep-peel patients with skin types III and IV with great results, but this is not for the beginner peeler,” she says.
Dr. Lee became involved with medical peels following a laser and cosmetic fellowship at Massachusetts General Hospital. “I started doing peels after I finished fellowship because finding the capital to invest in lasers—which is the area in which I was proficient—takes time. The startup cost for chemical peels is much more affordable and can give you similar results,” she says.
Today, many of her patients come to her practice for her expertise in deep and medium-depth peels. “A lot of patients come to me because they’ve already had a laser procedure and they didn’t get as much of a result as they were hoping for. Offering peels has differentiated my practice,” she says.
As with adding a new laser or energy-based device, deep chemical peels require training. “This is how we maintain patient safety and get good results,” says Dr. Lee. “The International Peeling Society (www.peelingsociety.com) is a great place to start with training.”
Inga Hansen is the executive editor of MedEsthetics.
Image copyright Getty Images