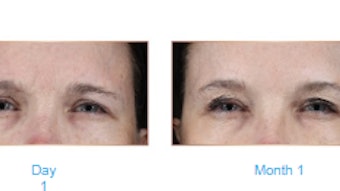
The use of calcium hydroxyapatite (CaHA) has continued to increase in popularity in cosmetic procedures, so authors Gurnam Virdi, M.D., and Emma Spotswood, RGN, suggested an exemplified protocol for managing life-changing complications of impending necrosis after injections with calcium hydroxyapatite.
Their case report, published in the Journal of Plastic and Reconstructive Surgery (May 2022), describes the successful management of impending skin necrosis after CaHA filler injections with a prompt diagnosis and management being paramount to prevent undesirable cosmetic outcomes.
Related: Guidelines to Manage CaHA Filler-related Intravascular Complications
The case report evaluated the treatment method that was taken on a 23-year-old female patient who received 1.5 ml of CaHA filler injections (Radiesse with lidocaine, Merz Aesthetics). While there were no signs of blanching, pain or skin discoloration at the time of treatment, the patient complained about severe pain, paraesthesia and paleness 12 hours later. An immediate face-to-face assessment revealed extensive livedo reticularis with capillary refill time delayed to six seconds in the mid-lower lip.
The treatment plan for this complication included:
- 300 mg of aspirin
- 600 units of hyaluronidase, injected away from the site of livedo reticularis every 45 minutes for a total of four rounds of treatment
- 5 ml of saline, injected away from the site of livedo reticularis
- 60 mg of oral steroids (prednisolone), with a tapering off regimen (60/40/40/20/10/10/5/5)
- 50 mg of sildenafil a day, taken for three days
- Low-molecular weight heparin, taken for seven days
- 200 mg doxycycline followed by a maintenance dose of 100 mg, given daily
- 200 mg acyclovir, given four times a day for seven days
- Two sessions of hyperbaric oxygen
After seven days, there were signs of dried debris and superficial necrotic tissue, so the wound was conservatively debrided to promote wound healing.
Related: Consensus Guidelines to Reduce the Risk of HA Filler Embolic Vision Loss
The key to managing vascular complications is rapid reperfusion of the affected area. A warm compress and vigorous massage promote vasodilation and may spread the filler distally into smaller arterioles. Despite the filler being resilient to the enzyme, hyaluronidase should be used due to its anti-inflammatory benefits and potential to reduce localized pressure. Virdi emphasizes the use of a cannula to administer the hyaluronidase to avoid masking crucial visual signs due to bruising.
Sound anatomical knowledge also plays a huge part in avoiding vascular complications. The submental artery is the largest cervical branch of the facial artery with an average diameter of 1.69 mm. It runs over the mylohyoid muscle, the mandible and ends in superficial and deep branches.
Related: Reducing Risks of HA Filler-induced Vascular Complications
The course of treatment detailed in this case report shows successful management of impending skin necrosis resulting from the submental artery after injection of CaHA filler. The key to treatment is a prompt diagnosis and management of the vascular compromised situation to avoid outcomes like scarring.